Introduction
With over 1,600,000 newly diagnosed patients each year, lung cancer is an extraordinarily heterogeneous illness and the acknowledged leading cause of the majority of cancer-related mortalities globally [1]. Non-small cell lung cancer (NSCLC), containing lung adenocarcinoma (LUAD) and lung squamous cell carcinoma (LUSC) [2], is the most common histological type of lung cancer, accounting for around 85% of all occurrences [3]. Despite tremendous advances in clinical screening and therapeutic therapies for NSCLC, the limited therapeutic benefit of first-line treatment resulted in a low overall cure and survival rate for NSCLC, particularly in metastatic disease. Despite tremendous advances in clinical screening and therapeutic therapies for NSCLC, the limited therapeutic benefit of first-line treatment resulted in a low overall cure and survival rate for NSCLC, particularly in metastatic disease [4]. As a result, additional research is needed to uncover more relevant biomarkers in order to extend clinical advantages to a larger patient population and enhance NSCLC outcomes.
Immunotherapy, which strengthens the patient’s immune system to fight malignancies, has received massive attention in recent years in the context of cancer treatment. Immunosurveillance, or the ability of immune cells in the tumor microenvironment (TME) to recognize and destroy cancer cells under normal conditions, is now widely acknowledged [5, 6]. Nevertheless, further investigation showed that cancer cells can control the host immune system to avoid immune monitoring by enlisting immunosuppressive cell populations and reducing the immunogenicity of tumors [7, 8]. In addition, tumors with different phenotype have distinct therapeutic responses. To be specific, hot tumors, featured by T-cell inflammation, showed a favorite therapeutic response to immunotherapy, while cold tumors are resistant to many treatments [9–12]. Thus, it is crucial to investigate the alteration of the TME to guide the personalized immunotherapy.
In the recent years, with the intensive investigation of different manners of cell death, numerous researchers found that anoikis is an important mechanism that can be introduced to treatment. Anoikis is a type of programmed cell death that takes place when cells separate from the proper extracellular matrix. This mechanism is essential for maintaining plastic cell development and attachment [13]. Notably, cancer cells are resistant to anoikis because they do not depend on extracellular matrix adherence for survival and growth [14], indicating that malignancies are a better example of anoikis resistance. Therefore, understanding the NSCLC anoikis regulators helps researchers find new treatments, particularly for cancer metastasis [15, 16]. For instance, through altering the JAK2/STAT3 and SHP2/Grb2 signaling pathways, the TGF-1/SH2B3 axis can control lung cancer cells’ anoikis resistance and EMT [17]. In addition, the enhancement of anoikis sensitivity could enhance immune cell-mediated cytotoxicity [18]. However, the association between anoikis and TME features in NSCLC is still unclear.
At present, several studies explored the correlation between the anoikis feature and immunological characteristics. Here, in this study, we first recognized the up-regulated anoikis-related genes (ARG) in NSCLC tumor tissues, and then construct a prognostic model based on these genes. Subsequently, we confirmed that the ARGs in the prognostic model were expressed on tumor cells at the single-cell level. Finally, further analysis was performed to explore the correlation between ARGs and immunological characteristics and the predictive value of ARGs model in immunotherapeutic response. Taken together, our study provided a new perspective to understand the clinical and immunological-related functions of ARGs, which contributes to the advancement of more precise and precise treatment strategies.
Materials and Methods
Data collection and processing
The gene expression matrices of NSCLC patients were downloaded from public online databases —the UCSC Xena website and the Gene Expression Omnibus (GEO) portal. The transcriptional omics and clinical annotations of tumors and paracancerous of NSCLC patients in the TCGA-LUAD and TCGA-LUSC cohorts were obtained from the UCSC Xena. In the GEO database, we identified three NSCLC cohorts (GSE30219 [19], GSE37745 [20], and GSE3141 [21]) with prognosis information. Besides, two clinical cohorts (GSE126044 [22] and GSE135222 [23]) of NSCLC patients received immunotherapy, were also obtained from the GEO database. Diagnostic patients with follow-up information, including survival outcomes or therapeutic responses were chosen for further analysis.
Assessment of biological functions
The R package “clusterProfiler” [26] was used to assess the biological functions of gene signatures in terms of Gene Ontology (GO) [27] and Kyoto Encyclopedia of Genes and Genomes (KEGG) [28] pathways. The top ten enriched pathways with the most significantly P-values were displayed.
Single-cell RNA sequencing datasets analysis
To further elaborate the tumor-specific of gene signatures in the prognostic model, single-cell RNA sequencing (scRNA-seq) datasets (GSE150660 [29] and GSE148071 [30]) were downloaded from the GEO protocol (All additional analyses were using the Seurat R toolkit [31].
For each sample, we summarized the expressed percentage of mitochondrial genes (percent.mt). Cells with percent.mt < 10% and 200 < nFeature_RNA < 5,000 were preserved. Then, for each dataset, the “RunHarmony” function [32] was applied to minimize the batch effects and integrate the transcriptional gene profiles from different patients. Principal component analysis (PCA) was performed based on the top 4,000 genes with highest variability. Then, the high dimensionality of data was reduced based on the top 30 PCs. The cells were unsupervised clustered via shared nearest neighbor (SNN) algorithm with one resolution. To annotate cell types, many well-known signatures were collected from previous studies [33, 34], such as EPCAM for tumor cells, CD3E for T cells, CD14 for macrophages, and CD1C for dendritic cells.
Cell-cell communication analysis
“CellPhoneDB” software [35] was utilized to deconstruct the cell-cell communications among cell types at the single cell level. To define the ARGRS+ and ARGRS- tumor cells, “AddModuleScore” function was applied to estimate the enrichment scores of the ARGRS based on the transcriptional level of the five genes in the model. Then, tumor cells with ARGRS > 0 were defined as ARGRS+ tumor cells, and other were ARGRS- tumor cells. The ligand-receptor pairs with P-value < 0.05 were included in further analysis.
Immune infiltration analysis
The gene signatures of immunomodulators, immune cell subpopulations and immunological signaling pathways were obtained from previous studies [36–38]. R package “estimate” was employed to examine the abundance of infiltrating immune cells (ImmuneScore) and tumor purity (TumorPurity). The R package “GSVA” (version 1.46.0) [39] was utilized to assess the enrichment scores of characteristics based on the gene signatures.
Clinical samples, immunohistochemistry, and quantitative evaluation
The NSCLC tissue microarray (TMA) section (HLugC120PT01) was obtained from Outdo Biotech (Shanghai, China). Ethical approval (YB-M-05-02) for the study of the TMA was granted by the Clinical Research Ethics Committee, Outdo Biotech (Shanghai, China). The TMA was used for immunohistochemistry (IHC) assay to measure the expression of HMGA1 protein in tumor and non-tumor breast tissues. IHC assay was performed on these sections according to the established steps. These sections were given three 5-minute xylene washes and rehydrated using a series of washes in ethanol grades of 70%, 90%, and 100%. For twenty minutes, endogenous peroxidase activity was inhibited using hydrogen peroxidase. The antigen retrieval solution is EDTA. The primary antibody utilized in the study was anti-HMGA1 (1:200 dilution, Cat. sc-393213, Santa Cruz) and anti-CD8A (ready-to-use, Cat. PA577, Abcarta). Antibody staining was visualized with DAB and hematoxylin counterstain. Using the immunoreactivity score standard, two senior pathologists assessed stained TMA to determine HMGA1 expression [40]. Two senior pathologists used The Cancer Genome Atlas Network’s criteria to determine the CD8 score for tumor-infiltrating CD8+ T cell assessment [41]. For every sample, a CD8 score, which is the total of the density and distribution scores (0–6), was determined. Samples classified as immune-cold are those with a CD8 score ≤ 2 (0, 2) and immune-hot samples with a score ≥ 3 (3, 4, 5, 6).
Statistical analysis
R-4.2.2 was used to perform all statistical analyses. The chi-square test was used to compare categorical variables, while the Wilcoxon rank-sum test was for continuous variables between the two groups. The log-rank test was used to assess the prognostic values. A two-paired p-value of less than 0.05 was considered statistically significant for all analyses, and the results were categorized as follows: *p-value < 0.05, **p-value ≤ 0.01, ***p-value ≤ 0.001, and ****p-value ≤ 0.0001.
Availability of data and materials
The TCGA data are openly available at https://portal.gdc.cancer.gov/, and the GEO data are openly available at https://www.ncbi.nlm.nih.gov/gds.
Consent for publication
All authors are consent for publication.
Results
Validation of the prognostic model in NSCLC
We further confirmed this finding in additional independent cohorts after discovering the prognostic predictive utility of ARGRS in the TCGA cohort. Patients in the GSE30219 cohort who had higher ARGRS had worse OS than those with lower ARGRS, which is consistent with the findings from the TCGA cohort (Figure 3A, 3B). ARGRS levels were also higher in patients with higher clinical stages and grades (Figure 3C), indicating its role in the malignancy of NSCLC. Patients in the ARGRS-high group similarly exhibited inferior clinical outcomes in the GSE37745 and the GSE3141 cohorts (Figure 3D, 3E). Based on the findings from the TCGA and additional independent cohorts, the ARGRS was linked to a worse OS for NSCLC patients and may have contributed to tumor progression.
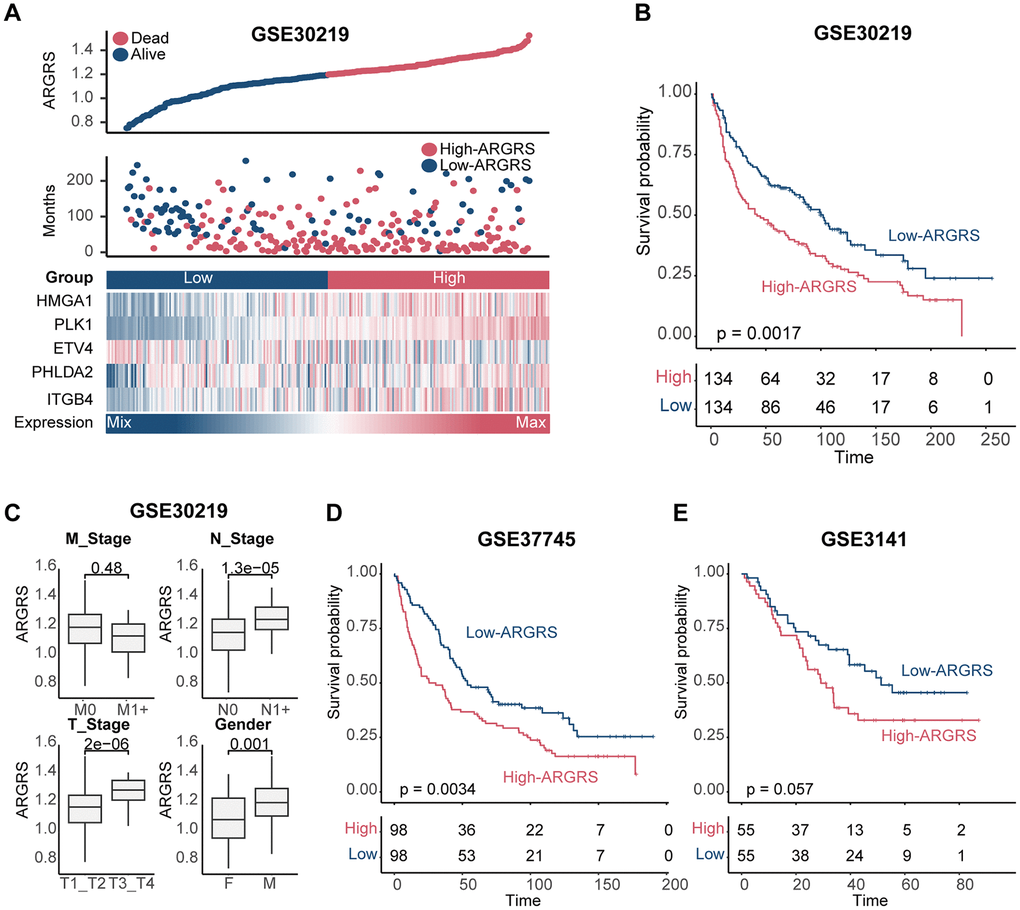
Figure 3. Validation of prognostic model in other independent cohorts. (A) Distributions of ARGRS, survival status of NSCLC patients, and expression profiles of the gene signatures in the GSE30219 cohort. (B) Survival analysis showing the prognostic value of ARGRS in the GSE30219 cohort. (C) Comparison of ARGRS among different clinicopathologic features. (D, E) Survival analysis showing the prognostic value of ARGRS in the (D) GSE37745 and (E) GSE3141 cohort.
Patients with higher ARGRS exhibit low immune infiltration
Having observed the existence of many immune cells in the NCLSC patients at the high dimensional datasets, we next explored the correlation between ARGRS and the fraction of each cell type. Notably, the ARGRS was negatively correlated with the fraction of T cells at the single-cell level (R2 = -0.93, p = 0.02, Figure 5A). Also, in the TCGA cohort, patients with higher ARGRS had lower levels of ImmuneScore but higher levels of tumor purity (Figure 5B), consistent with the results found in the single-cell datasets. In addition, a functional analysis of up-regulated genes in ARGRS-low group was highly related to immunological processes, such as cytokine activity, chemokine receptor binding and activity, and cytokine-cytokine receptor interaction (Figure 5C). Meanwhile, compared with the ARGRS-high group, the ARGRS-low group expressed higher transcriptional levels of immunological signatures, such as the biomarkers of CD8+T cells and NK (Figure 5D and Supplementary Figure 6). Also, the ARGRS-low group had higher fraction of CD8+T cells, and enriched some immune activation characteristics, such as the molecules of HLA, MHC, and immunostimulatory (Figure 5E, 5F). To be sum up, combined with the results found at the single-cell and omics transcriptional datasets, we found that ARGRS was negatively correlation with the fraction of T cells, and patients with the ARGRS-high phenotype exhibited low immune infiltration.
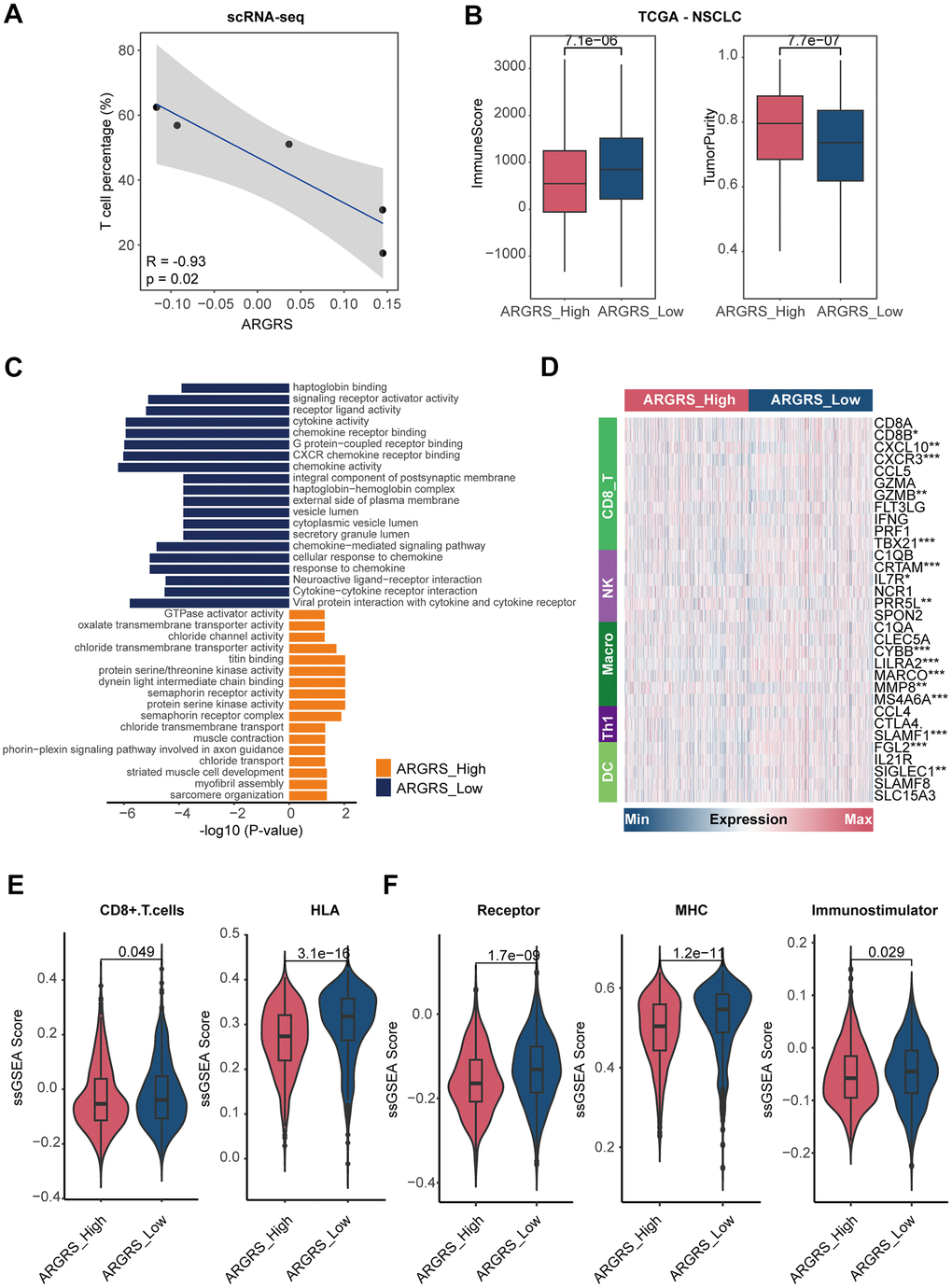
Figure 5. Patients with higher ARGRS exhibit low immune infiltration. (A) The correlation between the fraction of T cells and ARGRS levels at the single-cell level. X-axis: the fraction of T cells of each NSCLC patient. Y-axis: the median levels of ARGRS of each NSCLC patient. (B) Boxplot showing the levels of ImmuneScore (left) and TumorPurity (right) between the ARGRS-high and low groups in the TCGA NSCLC cohort. (C) GO and KEGG analyses of genes up-regulated in the ARGRS-high and low groups in the TCGA NSCLC cohort. (D) Heatmap showing the levels of immunological markers between ARGRS-high and low groups in the TCGA NSCLC cohort. (E, F) Comparison of immunological signatures between ARGRS-high and low groups in the TCGA NSCLC cohort.
In another independent cohort, we also found the similar results. ARGRS was negatively correlated with ImmuneScore (R2 = -0.32, p < 0.0001), but positively with tumor purity (R2 = 0.36, p < 0.0001, Supplementary Figure 7A–7C). Patients with the ARGRS-low phenotype had higher enrichment scores of immune-related characteristics, such as receptors and MHC molecules (Supplementary Figure 7D). Additionally, patients in the ARGRS- low groups also had higher levels of the immune-related signaling pathways and subpopulations (Supplementary Figure 7E), indicating activate immunological status of patients with the ARGRS- low phenotype. To further investigate the potential factors mediating the formation of inflamed or dessert TME, we deconstructed the interactions among cell populations. Results showed that compared with ARGRS- tumor cells, ARGRS+ tumor cells presented significantly more specific interactions with immune subpopulations (Supplementary Figure 8A). ARGRS+ tumor cells can communicate with T cell via many ligand-receptors (Supplementary Figure 8B), such as TIGIT-NECTIN2 [45] and LGALS9-CD44 [46], which were involved in suppressing tumor T cell infiltration, and promoted the cell state transition of immune cells towards a more immunosuppressive and exhaustive status, indicating the potential mechanism in mediating the dessert TME in the ARGRS-high group.
Patients with higher ARGRS were resistance to immunotherapy
Previous studies reported that the reactivity of immunotherapy was affected by the immunological status of patients. To be specific, hot tumors, featured by T-cell inflammation, were more sensitive to immunotherapies, while cold tumors are resistant to many treatments [9, 10]. Combined with the distinct immunological status between the ARGRS-high and low groups, the two groups may have different response of immunotherapy.
Here, to investigate the immunotherapeutic in the high- and ARGRS-low groups, we downloaded the expression matrix and clinical annotations of NSCLC patients in the cohorts received immunotherapy. In accordance with results above, ARGRS was negatively correlated with almost all immunological characteristics in the GSE126044 dataset (Figure 6A). Also, patients with the ARGRS-high phenotype had higher levels of ImmuneScore, but low tumor purity (Figure 6B, 6C). Besides, patients in the ARGRS-high group were centralized in the NR group (Figure 6D), indicating the immunotherapeutic resistance of them. Consistently, analysis of another immunotherapy cohort also showed the same results. Patients in the ARGRS-high group exhibit lower immune infiltration but higher tumor purity (Figure 6E–6G). Moreover, NSCLC patients in the ARGRS-high group were more likely to recurrence or progress after immunotherapy than the ARGRS-low group (Figure 6H), further supporting the immunotherapeutic resistance of them.
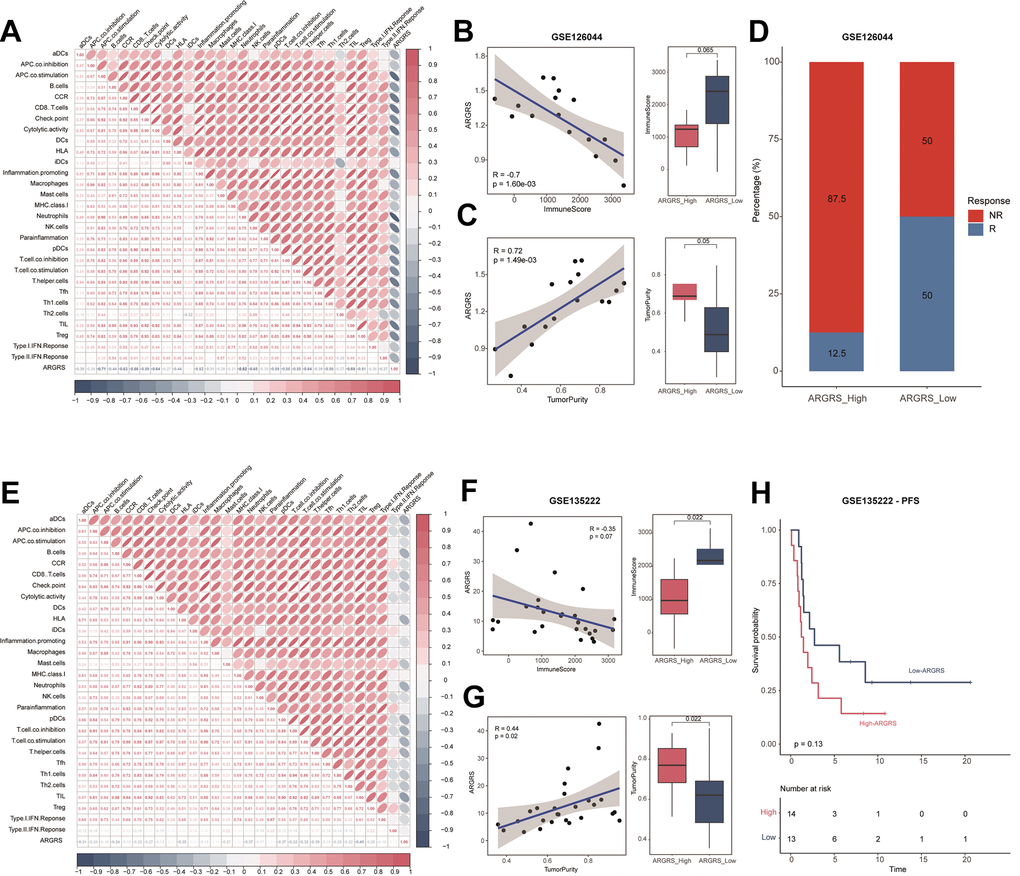
Figure 6. Patients with higher ARGRS were resistance to immunotherapy. (A) The correlation among 29 immune cell types and immune-related pathways and ARGRS in the GSE126044 cohort. (B) Left: Correlation between ARGRS and ImmuneScore in the GSE126044 cohort. Right: Boxplot showing the levels of ImmuneScore between ARGRS-high and low groups. (C) Left: Correlation between ARGRS and TumorPurity in the GSE126044 cohort. Right: Boxplot showing the levels of TumorPurity between ARGRS-high and low groups. (D) Barplot showing the percentage of immunotherapy responsive and non-responsive NSCLC patients in ARGRS-high and low groups. (E) The correlation among 29 immune cell types and immune-related pathways and ARGRS in the GSE135222 cohort. (F) Left: Correlation between ARGRS and ImmuneScore in the GSE135222 cohort. Right: Boxplot showing the levels of ImmuneScore between ARGRS-high and low groups. (G) Left: Correlation between ARGRS and TumorPurity in the GSE135222 cohort. Right: Boxplot showing the levels of TumorPurity between ARGRS-high and low groups. (H) Survival analysis showing the prognostic value of ARGRS in the GSE135222 cohort.
HMGA1 was the representative biomarker for NSCLC
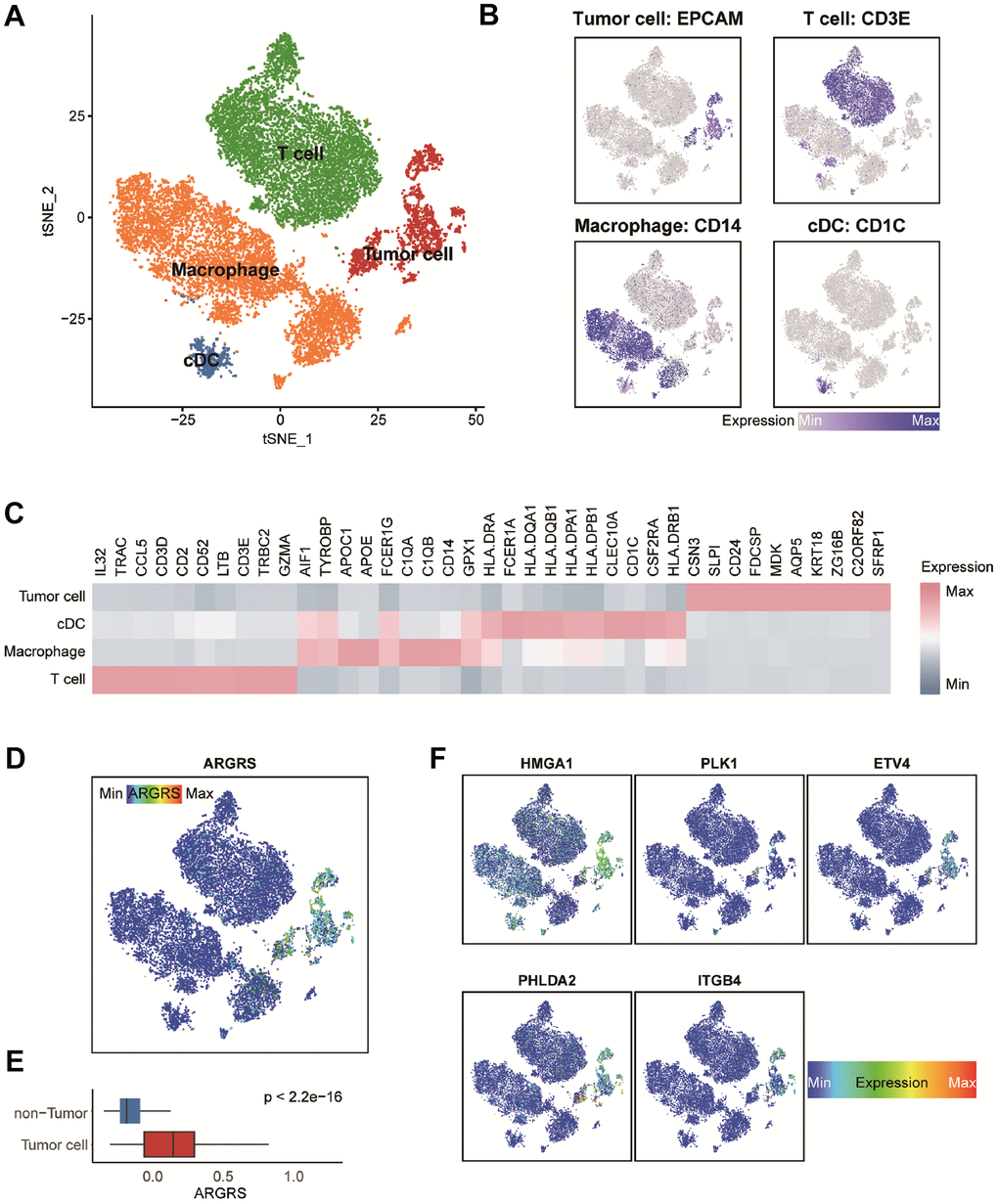
Next, we chose a representative biomarker from the five genes in the model for further experiments. Firstly, we summarized the expressed fraction of these genes at the single-cell levels. Compared with other genes in the model, tumor cells had obviously transcriptional levels and the highest expressed fraction of HMGA1 (Figure 7A, 7B, and Supplementary Figure 9A, 9B). Besides, at the high-resolution dataset, compared with other four genes, HMGA1 showed the most significant negative correlation with T cell inflamed and positive with tumor cells (Supplementary Figure 10). A Additionally, HMGA1 expressed was negatively correlated with ImmuneScore, but positively with tumor purity in multiple independent cohorts (Figure 7C–7F), suggesting the guidance of HMGA1 in distinguishing the hot and cold NSCLC tumors.
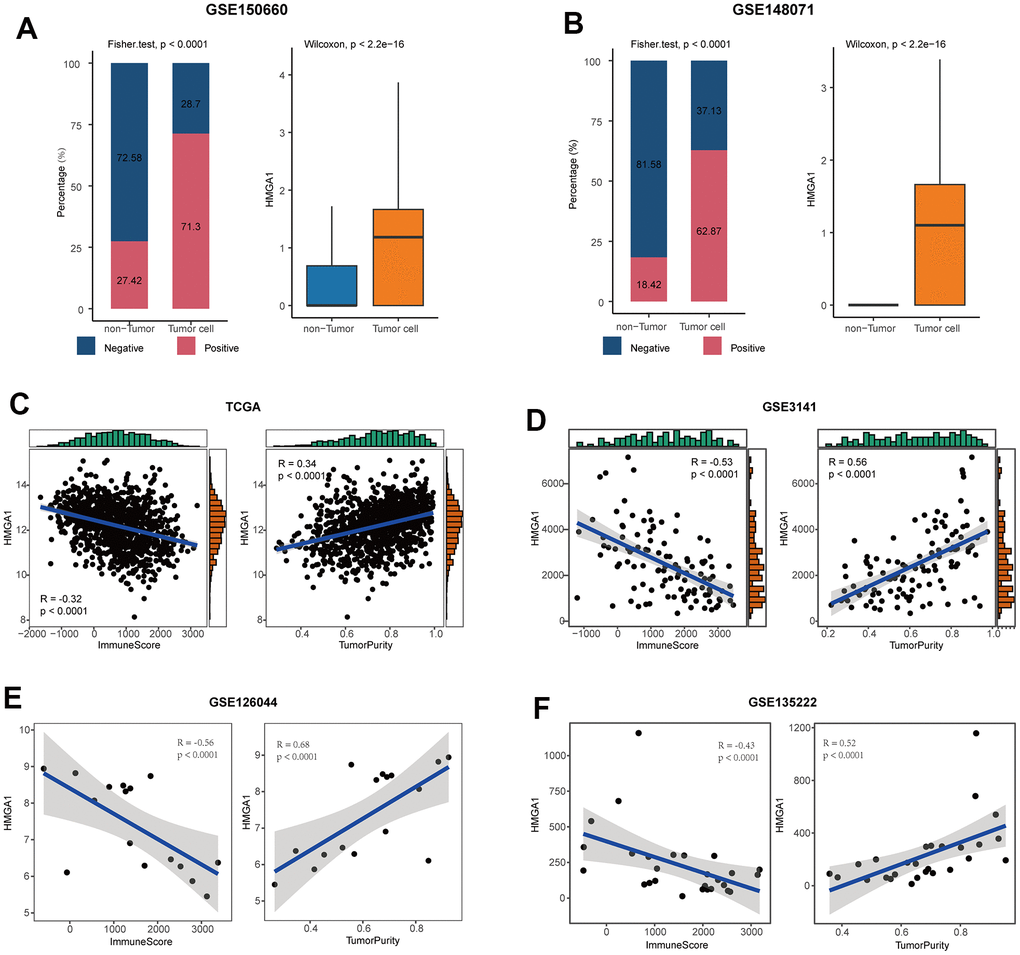
Figure 7. HMGA1 was the representative biomarker. (A) Right: bar plot showing the expressed fraction of HMGA1 between the non-tumor and tumor cells in the GSE150660 cohort. Left: comparison of the expression levels of HMGA1 between the non-tumor and tumor cells in the GSE150660 cohort. (B) Right: bar plot showing the expressed fraction of HMGA1 between the non-tumor and tumor cells in the GSE148071 cohort. Left: comparison of the expression levels of HMGA1 between the non-tumor and tumor cells in the GSE148071cohort. (C–F) Correlations between HMGA1 expression and ImmuneScore and tumor purity in (C) the TCGA, (D) the GSE3141, (E) the GSE126044, and (F) the GSE135222 cohorts.
Next, we verified the expression pattern of HMGA1 in the in-house cohort. We found that HMGA1 expression was significantly higher in tumor tissues than in para-tumor tissues (Figure 8A, 8B), and HMGA1 was specifically expressed in NSCLC (Figure 8C, 8D). We also classified NSCLC into immune-hot and cold tumors based on the CD8 scores. Besides, HMGA1 was significantly reduced in immune-hot tumors (Figure 8E, 8F) and negatively correlated with CD8 scores (Figure 8G). Overall, the negative correlation between HMGA1 expression and T cell infiltration can be verified in the in-house cohort, which greatly improves the confidence of the public cohort results.
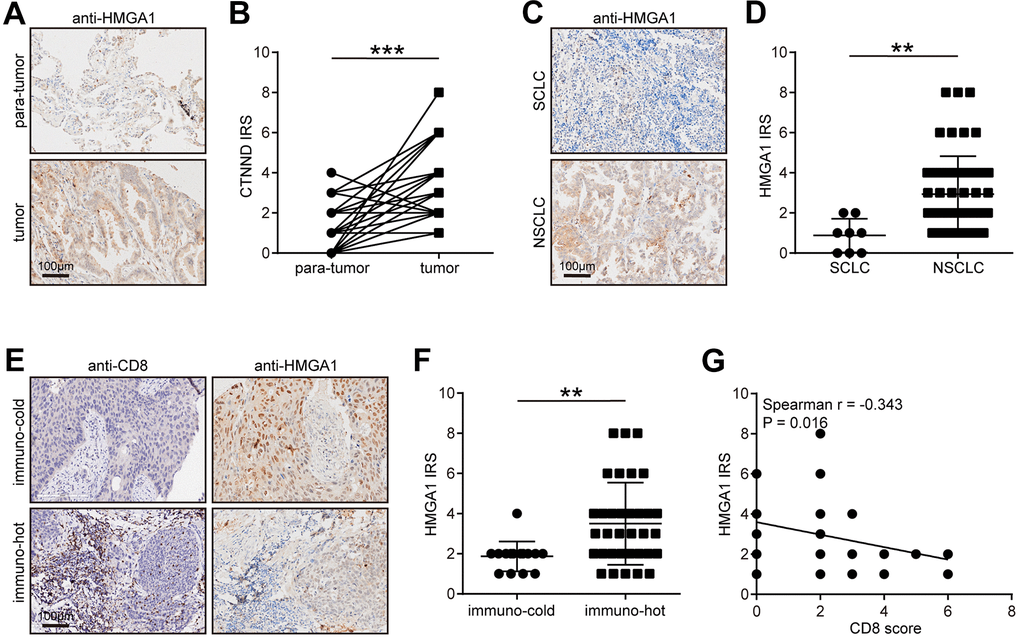
Figure 8. Validation of CTNND1 expression and its correlations with the TME features in the in-house cohort. (A, B) Representative images uncovering the expression of HMGA1 in para-tumor and tumor tissues and quantitative analysis. (C, D) Representative images uncovering the expression of HMGA1 in NSCLC and SCLC tumor tissues and quantitative analysis. (E, F) Representative images uncovering the expression of HMGA1 in immuno-cold and immuno-hot tumor tissues and quantitative analysis. (G) Correlation between HMGA1 expression and CD8 score.
Discussion
Nowadays, with the more profound of molecular and microenvironment characteristics of NSCLC, immunotherapy strategies, such as immune checkpoint inhibitors, has changed first-line treatment of advanced NSCLC, as we all know. Meanwhile, more than 10 indications for immunotherapies in NSCLC clinical practice has been approved by Chinese official organization [47–49].
Even while some patients have benefitted from this new therapy strategy in terms of survival, some individuals are still unable to get lasting relief. Tumor cell apoptosis can result in medication resistance, which in turn affects tumor cell survival in the bloodstream, which is essential for the development of metastasis. Jin et al. found that PLAG1 GDH1 axis promotes apoptotic resistance and tumor metastasis in LKB1-deficient malignancies via CamKK2 AMPK signaling pathway [50]. According to research, CPT1A-mediated fatty acid oxidation can encourage the spread of colorectal cancer cells by impairing the process of cell death [51]. Anoikis has been extensively investigated in relation to tumor growth and metastasis, but little is known about how it alters the tumor immune milieu and hence mediates tumor progression. We concentrate on the part anoikis play in the microenvironment of the tumor and investigate if anoikis can mediate the regulation of immunization, altering the growth and metastasis of the tumor.
We identified tumor-specific anoikis-related genes in NSCLC patients and used these genes to build a predictive model. Patients with higher ARGRS exhibited worse clinical outcomes, showing that ARGRS plays a role in the malignancy of NSCLC. Furthermore, using single-cell transcriptional datasets, we demonstrated that, when compared to non-tumor cells, tumor cells showed greater levels of ARGRS and signature expression in the prognostic model. Notably, ARGRS was negatively linked with the proportion of T cells at the single-cell level, meaning that ARGRS-high NSCLC patients were more likely to have the TME with minimal immune infiltration. Further investigation revealed that the results from the independent NSCLC cohorts were compatible with the findings at the high dimensionality datasets. Patients in the ARGRS-high group, in particular, showed lower levels of immune features but higher tumor purity.
Given of the important role of immunological status of TME in immunotherapeutic response [9, 10, 52], we further investigated the responses of the ARGRS-high and low groups in immunotherapy cohorts. Approximately 87.5% of patients in the ARGRS-high group did not achieve remission after immunotherapy, and were more likely to recurrence or progress, suggesting the immunotherapeutic resistance of these patients. There is now evidence that NSCLC patients can benefit from immunotherapy. However, limited by the inadequate research of characteristics to distinguish the inflamed and desert TME, numerous patients received immunotherapy without obtaining effective results. Therefore, we performed a comprehensive study on explore the ARGs and delved into the prognosis and immune microenvironment characteristics of NSCLC. Additionally, given the regulating upstream feature of ARGRS, targeting it can activate the patient’s immune system coincident with tumor cell killing.
In addition, we further validated the expression and immuno-correlations of HMGA1 in NSCLC in the in-house cohort. We found that HMGA1 was highly expressed in tumor tissues and enriched in immuno-cold tumors, indicating that HMGA1 could shape immuno-cold TME and promote immunosuppression. In fact, reversal of HMGA1-mediated immunosuppression could improve hepatocellular carcinoma therapy [53]. In the term of molecular mechanisms, HMGA1 acted as a crucial regulator of tumor-promoting macrophage recruitment by activating NF-κB-CCL2 signaling and also regulated PD-L1 expression to promote immunosuppression [54, 55].
Conclusions
In this study, we investigated NSCLC-specific anoikis-related genes and constructed a prognostic model. Patients with higher ARGRS had worse clinical outcomes. Besides, we proved that the ARGRS and signatures in the models were highly expressed on tumor cells, compared with the non-tumor cells at the single-cell level. Notably, we found that the ARGRS was negatively correlated with the fraction of T cells. And other independent cohorts also showed the same results. To be specific, the ARGRS-high group had low immune infiltration, while the ARGRS-low group showed more active immunological status. Furthermore, in the immunotherapy cohort, patients who did not achieve remission or had tumor progression after immunotherapy were enriched in the ARGRS-high group, suggesting that patients with the ARGRS-high phenotype were more likely to be resistant to immunotherapy. To sum up, we constructed an anoikis-related gene model, and explained the relationship between ARGRS and immunological status, which can help to develop more personalized and precise treatment strategies in clinical practice.
Supplementary Materials
Author Contributions
FW and LC designed the study and reviewed the data. YW, ZZ, QQ, and SX performed experiments and drafted the manuscript. YW, ZZ, and QQ performed bioinformatics analyses. All the authors have read, revised, and approved the manuscript.
Conflicts of Interest
The authors declare that they have no conflicts of interest.
Ethical Statement
Due to that the lung cancer tissue microarray was provided by Outdo BioTech Co. Ltd. (Shanghai, China, https://www.superchip.com.cn/), the Clinical Research Ethics Committee of Outdo BioTech approved the research of the TMAs (approval No. (YB-M-05-02).
Funding
This work was financially supported by the Key Project of Social Development in Jiangsu Province (BE2019691), the Project of Jiangsu Commission of Health (Z2020011), and the Postdoctoral Research Funding Project of Jiangsu Province (2021K012A).
References
- 1. Alberg AJ, Brock MV, Ford JG, Samet JM, Spivack SD. Epidemiology of lung cancer: Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest. 2013; 143:e1S–29S. https://doi.org/10.1378/chest.12-2345 [PubMed]
- 2. Relli V, Trerotola M, Guerra E, Alberti S. Abandoning the Notion of Non-Small Cell Lung Cancer. Trends Mol Med. 2019; 25:585–94. https://doi.org/10.1016/j.molmed.2019.04.012 [PubMed]
- 3. Mitchell PL, John T. Lung cancer in 2016: immunotherapy comes of age. Lancet Respir Med. 2016; 4:947–9. https://doi.org/10.1016/S2213-2600(16)30379-4 [PubMed]
- 4. Herbst RS, Morgensztern D, Boshoff C. The biology and management of non-small cell lung cancer. Nature. 2018; 553:446–54. https://doi.org/10.1038/nature25183 [PubMed]
- 5. Yu S, Li Y, Ren H, Zhou H, Ning Q, Chen X, Hu T, Yang L. PDK4 promotes tumorigenesis and cisplatin resistance in lung adenocarcinoma via transcriptional regulation of EPAS1. Cancer Chemother Pharmacol. 2021; 87:207–15. https://doi.org/10.1007/s00280-020-04188-9 [PubMed]
- 6. Kennedy LB, Salama AK. A review of cancer immunotherapy toxicity. CA Cancer J Clin. 2020; 70:86–104. https://doi.org/10.3322/caac.21596 [PubMed]
- 7. Jhunjhunwala S, Hammer C, Delamarre L. Antigen presentation in cancer: insights into tumour immunogenicity and immune evasion. Nat Rev Cancer. 2021; 21:298–312. https://doi.org/10.1038/s41568-021-00339-z [PubMed]
- 8. Xu J, Gao Z, Liu K, Fan Y, Zhang Z, Xue H, Guo X, Zhang P, Deng L, Wang S, Wang H, Wang Q, Zhao R, Li G. The Non-N6-Methyladenosine Epitranscriptome Patterns and Characteristics of Tumor Microenvironment Infiltration and Mesenchymal Transition in Glioblastoma. Front Immunol. 2022; 12:809808. https://doi.org/10.3389/fimmu.2021.809808 [PubMed]
- 9. Gajewski TF, Corrales L, Williams J, Horton B, Sivan A, Spranger S. Cancer Immunotherapy Targets Based on Understanding the T Cell-Inflamed Versus Non-T Cell-Inflamed Tumor Microenvironment. Adv Exp Med Biol. 2017; 1036:19–31. https://doi.org/10.1007/978-3-319-67577-0_2 [PubMed]
- 10. Hu R, Han Q, Zhang J. STAT3: A key signaling molecule for converting cold to hot tumors. Cancer Lett. 2020; 489:29–40. https://doi.org/10.1016/j.canlet.2020.05.035 [PubMed]
- 11. Mao W, Cai Y, Chen D, Jiang G, Xu Y, Chen R, Wang F, Wang X, Zheng M, Zhao X, Mei J. Statin shapes inflamed tumor microenvironment and enhances immune checkpoint blockade in non-small cell lung cancer. JCI Insight. 2022; 7:e161940. https://doi.org/10.1172/jci.insight.161940 [PubMed]
- 12. Mei J, Cai Y, Wang H, Xu R, Zhou J, Lu J, Yang X, Pan J, Liu C, Xu J, Zhu Y. Formin protein DIAPH1 positively regulates PD-L1 expression and predicts the therapeutic response to anti-PD-1/PD-L1 immunotherapy. Clin Immunol. 2023; 246:109204. https://doi.org/10.1016/j.clim.2022.109204 [PubMed]
- 13. Taddei ML, Giannoni E, Fiaschi T, Chiarugi P. Anoikis: an emerging hallmark in health and diseases. J Pathol. 2012; 226:380–93. https://doi.org/10.1002/path.3000 [PubMed]
- 14. Cai Q, Yan L, Xu Y. Anoikis resistance is a critical feature of highly aggressive ovarian cancer cells. Oncogene. 2015; 34:3315–24. https://doi.org/10.1038/onc.2014.264 [PubMed]
- 15. Sakamoto S, Kyprianou N. Targeting anoikis resistance in prostate cancer metastasis. Mol Aspects Med. 2010; 31:205–14. https://doi.org/10.1016/j.mam.2010.02.001 [PubMed]
- 16. Yu Y, Song Y, Cheng L, Chen L, Liu B, Lu D, Li X, Li Y, Lv F, Xing Y. CircCEMIP promotes anoikis-resistance by enhancing protective autophagy in prostate cancer cells. J Exp Clin Cancer Res. 2022; 41:188. https://doi.org/10.1186/s13046-022-02381-7 [PubMed]
- 17. Wang LN, Zhang ZT, Wang L, Wei HX, Zhang T, Zhang LM, Lin H, Zhang H, Wang SQ. TGF-β1/SH2B3 axis regulates anoikis resistance and EMT of lung cancer cells by modulating JAK2/STAT3 and SHP2/Grb2 signaling pathways. Cell Death Dis. 2022; 13:472. https://doi.org/10.1038/s41419-022-04890-x [PubMed]
- 18. Ahn HM, Ryu J, Song JM, Lee Y, Kim HJ, Ko D, Choi I, Kim SJ, Lee JW, Kim S. Anti-cancer Activity of Novel TM4SF5-Targeting Antibodies through TM4SF5 Neutralization and Immune Cell-Mediated Cytotoxicity. Theranostics. 2017; 7:594–613. https://doi.org/10.7150/thno.15629 [PubMed]
- 19. Rousseaux S, Debernardi A, Jacquiau B, Vitte AL, Vesin A, Nagy-Mignotte H, Moro-Sibilot D, Brichon PY, Lantuejoul S, Hainaut P, Laffaire J, de Reyniès A, Beer DG, et al. Ectopic activation of germline and placental genes identifies aggressive metastasis-prone lung cancers. Sci Transl Med. 2013; 5:186ra66. https://doi.org/10.1126/scitranslmed.3005723 [PubMed]
- 20. Botling J, Edlund K, Lohr M, Hellwig B, Holmberg L, Lambe M, Berglund A, Ekman S, Bergqvist M, Pontén F, König A, Fernandes O, Karlsson M, et al. Biomarker discovery in non-small cell lung cancer: integrating gene expression profiling, meta-analysis, and tissue microarray validation. Clin Cancer Res. 2013; 19:194–204. https://doi.org/10.1158/1078-0432.CCR-12-1139 [PubMed]
- 21. Bild AH, Yao G, Chang JT, Wang Q, Potti A, Chasse D, Joshi MB, Harpole D, Lancaster JM, Berchuck A, Olson JA
Jr , Marks JR, Dressman HK, et al. Oncogenic pathway signatures in human cancers as a guide to targeted therapies. Nature. 2006; 439:353–7. https://doi.org/10.1038/nature04296 [PubMed] - 22. Cho JW, Hong MH, Ha SJ, Kim YJ, Cho BC, Lee I, Kim HR. Genome-wide identification of differentially methylated promoters and enhancers associated with response to anti-PD-1 therapy in non-small cell lung cancer. Exp Mol Med. 2020; 52:1550–63. https://doi.org/10.1038/s12276-020-00493-8 [PubMed]
- 23. Jung H, Kim HS, Kim JY, Sun JM, Ahn JS, Ahn MJ, Park K, Esteller M, Lee SH, Choi JK. DNA methylation loss promotes immune evasion of tumours with high mutation and copy number load. Nat Commun. 2019; 10:4278. https://doi.org/10.1038/s41467-019-12159-9 [PubMed]
- 24. Rebhan M, Chalifa-Caspi V, Prilusky J, Lancet D. GeneCards: integrating information about genes, proteins and diseases. Trends Genet. 1997; 13:163. https://doi.org/10.1016/s0168-9525(97)01103-7 [PubMed]
- 25. Rouillard AD, Gundersen GW, Fernandez NF, Wang Z, Monteiro CD, McDermott MG, Ma’ayan A. The harmonizome: a collection of processed datasets gathered to serve and mine knowledge about genes and proteins. Database (Oxford). 2016; 2016:baw100. https://doi.org/10.1093/database/baw100 [PubMed]
- 26. Yu G, Wang LG, Han Y, He QY. clusterProfiler: an R package for comparing biological themes among gene clusters. OMICS. 2012; 16:284–7. https://doi.org/10.1089/omi.2011.0118 [PubMed]
- 27. Gene Ontology Consortium. Gene Ontology Consortium: going forward. Nucleic Acids Res. 2015; 43:D1049–56. https://doi.org/10.1093/nar/gku1179 [PubMed]
- 28. Kanehisa M, Goto S. KEGG: kyoto encyclopedia of genes and genomes. Nucleic Acids Res. 2000; 28:27–30. https://doi.org/10.1093/nar/28.1.27 [PubMed]
- 29. Chi Y, Remsik J, Kiseliovas V, Derderian C, Sener U, Alghader M, Saadeh F, Nikishina K, Bale T, Iacobuzio-Donahue C, Thomas T, Pe’er D, Mazutis L, Boire A. Cancer cells deploy lipocalin-2 to collect limiting iron in leptomeningeal metastasis. Science. 2020; 369:276–82. https://doi.org/10.1126/science.aaz2193 [PubMed]
- 30. Wu F, Fan J, He Y, Xiong A, Yu J, Li Y, Zhang Y, Zhao W, Zhou F, Li W, Zhang J, Zhang X, Qiao M, et al. Single-cell profiling of tumor heterogeneity and the microenvironment in advanced non-small cell lung cancer. Nat Commun. 2021; 12:2540. https://doi.org/10.1038/s41467-021-22801-0 [PubMed]
- 31. Butler A, Hoffman P, Smibert P, Papalexi E, Satija R. Integrating single-cell transcriptomic data across different conditions, technologies, and species. Nat Biotechnol. 2018; 36:411–20. https://doi.org/10.1038/nbt.4096 [PubMed]
- 32. Korsunsky I, Millard N, Fan J, Slowikowski K, Zhang F, Wei K, Baglaenko Y, Brenner M, Loh PR, Raychaudhuri S. Fast, sensitive and accurate integration of single-cell data with Harmony. Nat Methods. 2019; 16:1289–96. https://doi.org/10.1038/s41592-019-0619-0 [PubMed]
- 33. Li Q, Wang R, Yang Z, Li W, Yang J, Wang Z, Bai H, Cui Y, Tian Y, Wu Z, Guo Y, Xu J, Wen L, et al. Molecular profiling of human non-small cell lung cancer by single-cell RNA-seq. Genome Med. 2022; 14:87. https://doi.org/10.1186/s13073-022-01089-9 [PubMed]
- 34. Mei J, Cai Y, Chen L, Wu Y, Liu J, Qian Z, Jiang Y, Zhang P, Xia T, Pan X, Zhang Y. The heterogeneity of tumour immune microenvironment revealing the CRABP2/CD69 signature discriminates distinct clinical outcomes in breast cancer. Br J Cancer. 2023; 129:1645–57. https://doi.org/10.1038/s41416-023-02432-6 [PubMed]
- 35. Efremova M, Vento-Tormo M, Teichmann SA, Vento-Tormo R. CellPhoneDB: inferring cell-cell communication from combined expression of multi-subunit ligand-receptor complexes. Nat Protoc. 2020; 15:1484–506. https://doi.org/10.1038/s41596-020-0292-x [PubMed]
- 36. Cai Y, Ji W, Sun C, Xu R, Chen X, Deng Y, Pan J, Yang J, Zhu H, Mei J. Interferon-Induced Transmembrane Protein 3 Shapes an Inflamed Tumor Microenvironment and Identifies Immuno-Hot Tumors. Front Immunol. 2021; 12:704965. https://doi.org/10.3389/fimmu.2021.704965 [PubMed]
- 37. Mei J, Fu Z, Cai Y, Song C, Zhou J, Zhu Y, Mao W, Xu J, Yin Y. SECTM1 is upregulated in immuno-hot tumors and predicts immunotherapeutic efficacy in multiple cancers. iScience. 2023; 26:106027. https://doi.org/10.1016/j.isci.2023.106027 [PubMed]
- 38. Mei J, Cai Y, Xu R, Zhu Y, Zhao X, Zhang Y, Mao W, Xu J, Yin Y. Protocol to identify novel immunotherapy biomarkers based on transcriptomic data in human cancers. STAR Protoc. 2023; 4:102258. https://doi.org/10.1016/j.xpro.2023.102258 [PubMed]
- 39. Hänzelmann S, Castelo R, Guinney J. GSVA: gene set variation analysis for microarray and RNA-seq data. BMC Bioinformatics. 2013; 14:7. https://doi.org/10.1186/1471-2105-14-7 [PubMed]
- 40. Mei J, Liu Y, Yu X, Hao L, Ma T, Zhan Q, Zhang Y, Zhu Y. YWHAZ interacts with DAAM1 to promote cell migration in breast cancer. Cell Death Discov. 2021; 7:221. https://doi.org/10.1038/s41420-021-00609-7 [PubMed]
- 41. Cancer Genome Atlas Network. Genomic Classification of Cutaneous Melanoma. Cell. 2015; 161:1681–96. https://doi.org/10.1016/j.cell.2015.05.044 [PubMed]
- 42. Mezquita L, Jové M, Nadal E, Kfoury M, Morán T, Ricordel C, Dhooge M, Tlemsani C, Léna H, Teulé A, Álvarez JV, Raimbourg J, Hiret S, et al. High Prevalence of Somatic Oncogenic Driver Alterations in Patients With NSCLC and Li-Fraumeni Syndrome. J Thorac Oncol. 2020; 15:1232–9. https://doi.org/10.1016/j.jtho.2020.03.005 [PubMed]
- 43. Offin M, Chan JM, Tenet M, Rizvi HA, Shen R, Riely GJ, Rekhtman N, Daneshbod Y, Quintanal-Villalonga A, Penson A, Hellmann MD, Arcila ME, Ladanyi M, et al. Concurrent RB1 and TP53 Alterations Define a Subset of EGFR-Mutant Lung Cancers at risk for Histologic Transformation and Inferior Clinical Outcomes. J Thorac Oncol. 2019; 14:1784–93. https://doi.org/10.1016/j.jtho.2019.06.002 [PubMed]
- 44. Jamme P, Fernandes M, Copin MC, Descarpentries C, Escande F, Morabito A, Grégoire V, Jamme M, Baldacci S, Tulasne D, Kherrouche Z, Cortot AB. Alterations in the PI3K Pathway Drive Resistance to MET Inhibitors in NSCLC Harboring MET Exon 14 Skipping Mutations. J Thorac Oncol. 2020; 15:741–51. https://doi.org/10.1016/j.jtho.2020.01.027 [PubMed]
- 45. Ho DW, Tsui YM, Chan LK, Sze KM, Zhang X, Cheu JW, Chiu YT, Lee JM, Chan AC, Cheung ET, Yau DT, Chia NH, Lo IL, et al. Single-cell RNA sequencing shows the immunosuppressive landscape and tumor heterogeneity of HBV-associated hepatocellular carcinoma. Nat Commun. 2021; 12:3684. https://doi.org/10.1038/s41467-021-24010-1 [PubMed]
- 46. Yang R, Sun L, Li CF, Wang YH, Yao J, Li H, Yan M, Chang WC, Hsu JM, Cha JH, Hsu JL, Chou CW, Sun X, et al. Galectin-9 interacts with PD-1 and TIM-3 to regulate T cell death and is a target for cancer immunotherapy. Nat Commun. 2021; 12:832. https://doi.org/10.1038/s41467-021-21099-2 [PubMed]
- 47. Liu L, Bai H, Wang C, Seery S, Wang Z, Duan J, Li S, Xue P, Wang G, Sun Y, Du X, Zhang X, Ma Z, Wang J. Efficacy and Safety of First-Line Immunotherapy Combinations for Advanced NSCLC: A Systematic Review and Network Meta-Analysis. J Thorac Oncol. 2021; 16:1099–117. https://doi.org/10.1016/j.jtho.2021.03.016 [PubMed]
- 48. Vaddepally RK, Kharel P, Pandey R, Garje R, Chandra AB. Review of Indications of FDA-Approved Immune Checkpoint Inhibitors per NCCN Guidelines with the Level of Evidence. Cancers (Basel). 2020; 12:738. https://doi.org/10.3390/cancers12030738 [PubMed]
- 49. Wang Y, Liu JJ, Dransfield PJ, Zhu L, Wang Z, Du X, Jiao X, Su Y, Li AR, Brown SP, Kasparian A, Vimolratana M, Yu M, et al. Discovery and Optimization of Potent GPR40 Full Agonists Containing Tricyclic Spirocycles. ACS Med Chem Lett. 2013; 4:551–5. https://doi.org/10.1021/ml300427u [PubMed]
- 50. Jin L, Chun J, Pan C, Kumar A, Zhang G, Ha Y, Li D, Alesi GN, Kang Y, Zhou L, Yu WM, Magliocca KR, Khuri FR, et al. The PLAG1-GDH1 Axis Promotes Anoikis Resistance and Tumor Metastasis through CamKK2-AMPK Signaling in LKB1-Deficient Lung Cancer. Mol Cell. 2018; 69:87–99.e7. https://doi.org/10.1016/j.molcel.2017.11.025 [PubMed]
- 51. Wang YN, Zeng ZL, Lu J, Wang Y, Liu ZX, He MM, Zhao Q, Wang ZX, Li T, Lu YX, Wu QN, Yu K, Wang F, et al. CPT1A-mediated fatty acid oxidation promotes colorectal cancer cell metastasis by inhibiting anoikis. Oncogene. 2018; 37:6025–40. https://doi.org/10.1038/s41388-018-0384-z [PubMed]
- 52. Mei J, Cai Y, Xu R, Yu X, Han X, Weng M, Chen L, Ma T, Gao T, Gao F, Xia T, Zhu Y, Zhang Y. Angiotensin-converting enzyme 2 identifies immuno-hot tumors suggesting angiotensin-(1-7) as a sensitizer for chemotherapy and immunotherapy in breast cancer. Biol Proced Online. 2022; 24:15. https://doi.org/10.1186/s12575-022-00177-9 [PubMed]
- 53. Yan B, Liu C, Li H, Wen N, Jiao W, Wang S, Zhang Y, Zhang T, Zhang H, Lv Y, Fan H, Liu X. Reversal of HMGA1-Mediated Immunosuppression Synergizes with Immunogenic Magnetothermodynamic for Improved Hepatocellular Carcinoma Therapy. ACS Nano. 2023; 17:9209–23. https://doi.org/10.1021/acsnano.3c00004 [PubMed]
- 54. Chang X, Liu J, Yang Q, Gao Y, Ding X, Zhao J, Li Y, Liu Z, Li Z, Wu Y, Zuo D. Targeting HMGA1 contributes to immunotherapy in aggressive breast cancer while suppressing EMT. Biochem Pharmacol. 2023; 212:115582. https://doi.org/10.1016/j.bcp.2023.115582 [PubMed]
- 55. Chen J, Ji K, Gu L, Fang Y, Pan M, Tian S. HMGA1 Promotes Macrophage Recruitment via Activation of NF-κB-CCL2 Signaling in Hepatocellular Carcinoma. J Immunol Res. 2022; 2022:4727198. https://doi.org/10.1155/2022/4727198 [PubMed]