Introduction
Pancreatic cancer is one of the most lethal malignancies in the world, with a high death rate and poor prognosis [1]. Annually, there are approximately 57,600 newly diagnosed cases of pancreatic cancer, with 47,050 deaths [2]. Pancreatic cancer survival rates remain low compared with those of other malignancies despite improvements in diagnostic and therapeutic techniques [3]. Therefore, it is increasingly necessary to develop new prognostic indicators that accurately predict the patient’s prognosis and guide treatment.
Protein glycosylation is one of the most important post-translational modifications of proteins. It involves carbohydrate transfer to proteins by glycosyltransferases and glycosidases [4–7]. Glycosylation is generally classified as N-linked or O-linked. N-glycosylation occurs when glycans from lipid-linked oligosaccharides are transferred to asparagine residues in the protein [8], while O-glycosylation occurs when glycans are linked to the hydroxyl groups of serine or threonine residues [9]. N-glycans contain three mannose and two N-acetylglucosamine (GlcNAc) subunits as the common pentasaccharides; this can be modified by adding galactose, GlcNAc, fucose, and sialic acid moieties [10].
Glycosylation aberrations are proposed hallmarks of most cancers [11]. Glycosylation regulates key steps of cancer biology, including tumor invasion, metastasis, and cellular signaling [12–15]. Moreover, abnormal glycosylation is an important indicator to induce tumor immune regulation because it provides recognition antigens for T cells [11, 16]. Abnormal glycosylation patterns identified in pancreatic cancer include O-GlcNAc, sialylation, aberrant branching, O-glycan structures, fucosylation, and altered mucins [17]. This alters multiple tumor-promoting signaling pathways, augments metastatic phenotypes, and remodels the tumor immune microenvironment [18].
Several prognostic models for pancreatic cancer were developed using post-translational regulatory biomarkers, including alternative splicing [19] and N6-methyladenosine modification [20]. Despite being a prominent hallmark of over 300 post-translational modifications [21], no systematic research has been conducted on the relationship between glycosylation and pancreatic cancer. This study developed a glycosylation-based three-gene prognostic model in pancreatic cancer and demonstrated its predictive ability.
Results
Determination of pancreatic cancer subtypes using DE-GRGs
TCGA-pancreatic cancer samples were divided into four clusters (group 1 (C1), group 2 (C2), group 3 (C3), and group 4 (C4)) based on 12 DE-GRGs (Figure 2A–2D). Kaplan–Meier plots showed significant survival disparities between these four groups, group C4 had the worst prognosis and group C2 had the best prognosis (Figure 2E). Further analysis was conducted on the distribution of the tumor, node, and metastasis (TNM) stage and pathological grade among the four subgroups. The samples in cluster-1 showed higher T classifications, but low clinical stage and histological grade; cluster-2 had higher N classification, clinical stage, and pathological grade; cluster-3 had higher N classification, but lower clinical stage and histological grade; and cluster-4 had lower T classification, N classification, clinical stage, and histological grade (Figure 3).
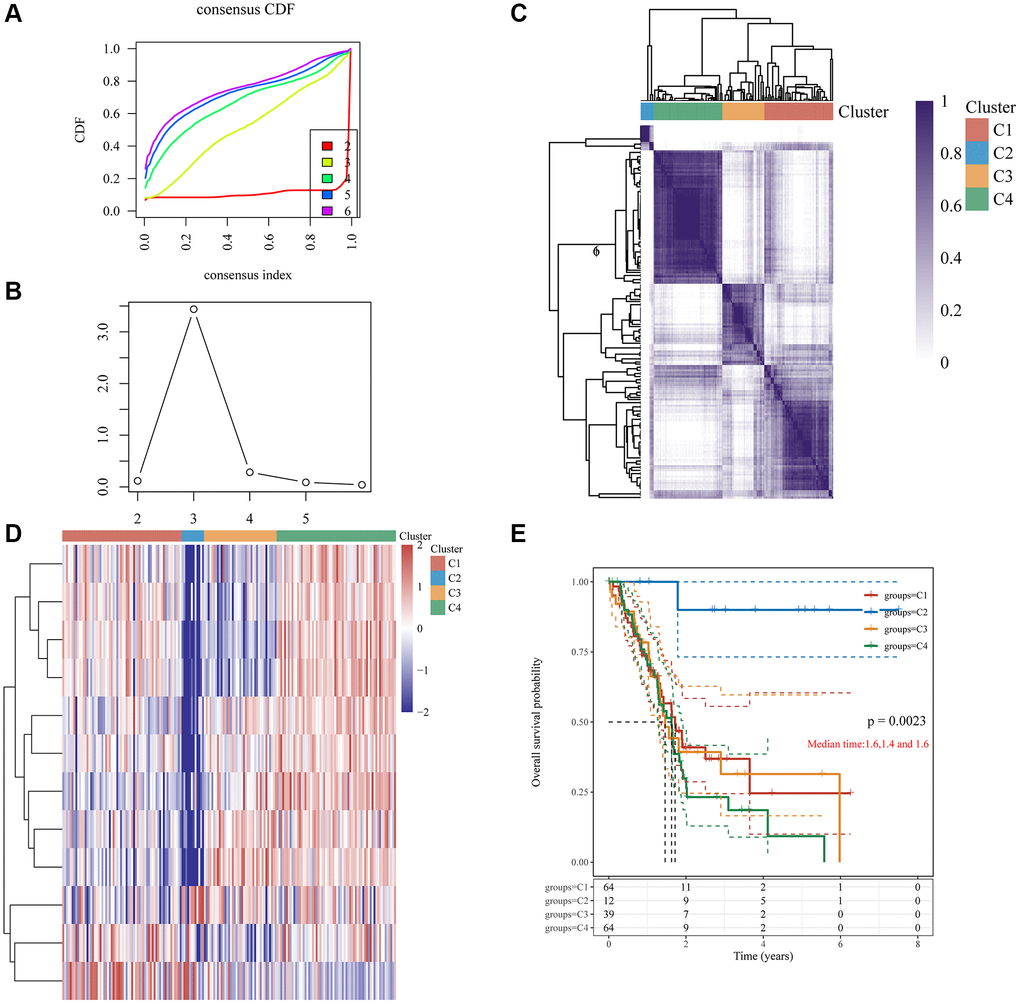
Figure 2. Clustering of PC molecular subgroups based on 12 GRGs. (A) Cumulative distribution function (CDF) curve. (B) CDF delta area curve, which shows how the area under the CDF curve changes between k and k-1 for each category number. The horizontal axis represents the number k, and the vertical axis represents the change in area under the CDF curve; each line represents a relative change. (C) A heatmap representing the consensus matrix for k = 4 derived from consensus clustering. Rows and columns in the matrix represent samples, and the degrees of consistency are represented by white to dark blue. (D) The heatmap of 12 GRGs in 4 clusters. (E) The KM survival curve of different groups in TCGA data sets.
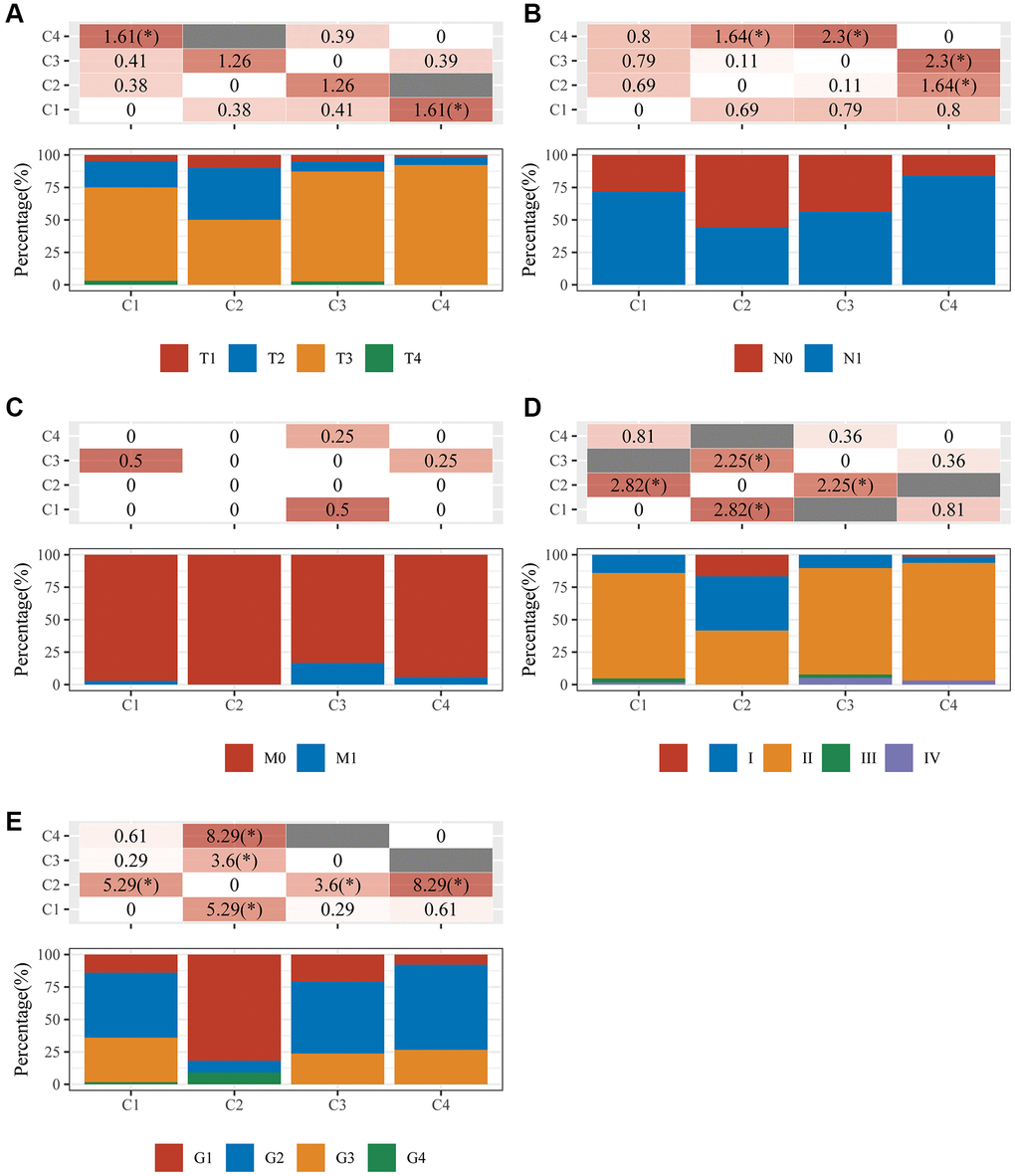
Figure 3. An analysis of clinical characteristics in four clusters. The horizontal axis represents the different sample groups. The vertical axis indicates how much clinical information is present in each grouped sample. The table above shows the clinical feature significance p-value (-log10) (based on the chi-square test). (A) T staging; (B) N staging; (C) M staging; (D) clinical stage; (E) clinical grade.
C1, C2, C3, and C4 immune status and stemness
Immunedeconv (combining CIBERSORT, EPIC, MCP-counter, quanTIseq, TIMER, and xCell software) was used to assess the immune infiltration among these four groups [22]. This analysis used the most widely used algorithm, CIBERSORT [23]. There were significant differences in the counts of CD8+ T cells (p < 0.001), regulatory T cells (Tregs) (p < 0.05), memory B cells (p < 0.01), resting natural killer (NK) cells (p < 0.05), activated NK cells (p < 0.05), monocytes (p < 0.05), M0 macrophages (p < 0.001), M1 macrophages (p < 0.05), and neutrophils (p < 0.05) (Figure 4A). Additionally, the R software tools ggplot2 and pheatmap were used to analyze the four immune checkpoint gene subtypes (ICGs) and significant differences were discovered between them (all p < 0.01, Figure 4B). The TIDE algorithm was used to predict cancer immune responses [22]. Clusters C1 and C4 performed better than clusters C2 and C3 (all p < 0.05, Figure 4C). This finding indicates that clusters C2 and C3 might achieve more clinical benefit following ICBs. Finally, examination of the mRNA stemness index (mRNAsi) levels of the four subtypes using the one-class logistic regression (OCLR) algorithm [24] revealed significant differences between clusters C1 and C2 (p < 0.01), C1 and C3 (p < 0.0001), C2 and C4 (p < 0.001), and C3 and C4 (p < 0.0001) (Figure 4D).
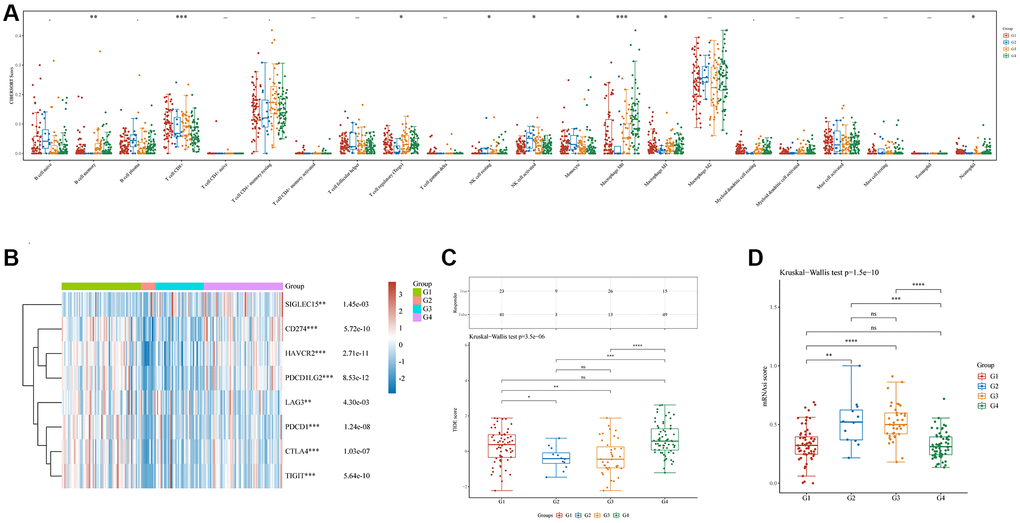
Figure 4. Immune and stemness analysis in four clusters. (A) Analysis of immune infiltration by C1, C2, C3, and C4 based on the CIBERSORT algorithm; the horizontal axis represents immune cells, while the vertical axis displays immune scores (*p < 0.05, **p < 0.01, ***p < 0.001). (B) Comparison of immune-checkpoint gene expression in C1, C2, C3, and C4; the horizontal axis shows different immune checkpoint genes, while the vertical axis displays the expression level (*p < 0.05, **p < 0.01, ***p < 0.001). (C) A statistical table showing the immune response and the distribution of scores for the different groups, according to the prediction. (D) A comparison of stemness for C1, C2, C3, and C4 using mRNAsi scores and the OCLR algorithm.
A prognostic nomogram that uses prognostic signatures from TCGA to predict overall survival in pancreatic cancer cohorts
Age and risk-score based prognostic signatures were independent risk factors for OS of pancreatic cancer using univariate and multivariate Cox regression analyses (p < 0.05) (Figure 7A, 7B). These two factors were integrated to develop a nomogram for overall survival prediction (Figure 7C). The regression coefficients for each influencing factor were added to obtain the total score. The overall score was converted to the probability that each outcome would occur to calculate the predicted value of each outcome. There was a better correlation between the nomogram predictions and actual survival rates for the first, third, and fifth years based on calibration plots (Figure 7D).
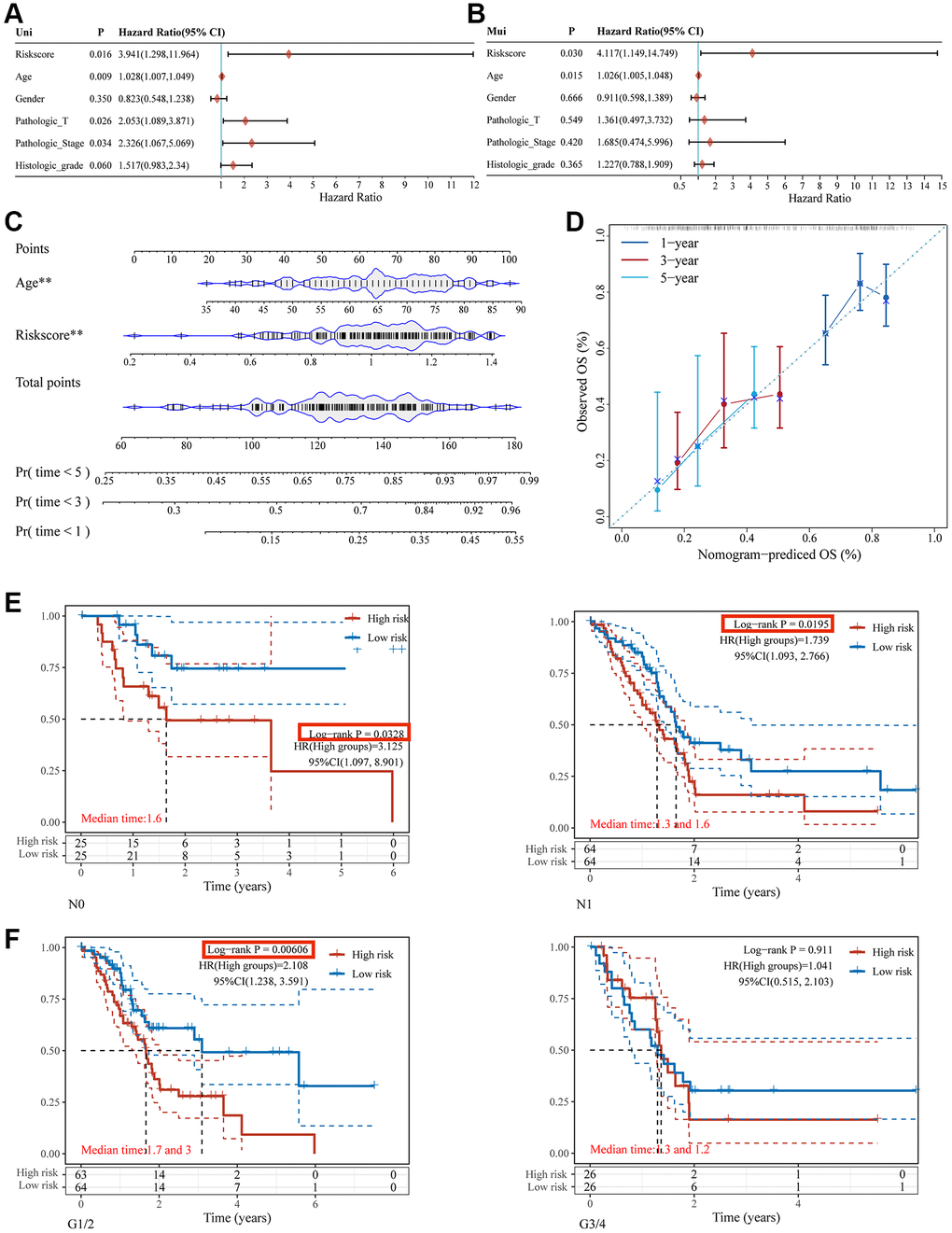
Figure 7. Nomogram construction for patients with PC in the TCGA database. The forest plot of the univariate (A) and multivariate (B) association between risk scores and clinicopathological characteristics. (C) A nomogram based on two independent prognostic factors was developed to predict the OS in patients with PC over 1, 3, and 5 years. (D) The calibration plot for internal validation of the nomogram. Survival analyses using the glycosylation-related signature in patients with different N staging (E) and clinical grade (F).
The relationship between SEL1L, TUBA1C, and SDC1 expression and clinical features
As mentioned above, glycosylation-related signatures based on three GRGs (SEL1L, TUBA1C, and SDC1) were affected by various clinical features. We classified pancreatic cancer patients into subgroups based on age (<45 or >45), sex (male or female), grade (G1, 2, 3, or 4), T stage (T1/2 or T3/4), N staging (N0 or N1), M stage (M0 or M1), clinical stage (I, II, III, or IV), chemotherapy (yes or no), and radiotherapy (yes or no), and compared the expression levels of SEL1L/TUBA1C/SDC1 between them. There was an insignificant correlation between the GRGs and age (Figure 9A) or sex (Figure 9B). High expression of TUBA1C and SDC1 was negatively correlated with grade (Figure 9C). No significant results were observed between the GRGs and clinical stage (Figure 9D). High TUBA1C expression positively correlated with T staging (Figure 9E), and N staging (Figure 9F) and M staging (Figure 9G) were adversely linked with high expression of SEL1L. Similarly, there was no correlation between the expression of GRGs and chemotherapy (Figure 9H) or radiotherapy (Figure 9I).
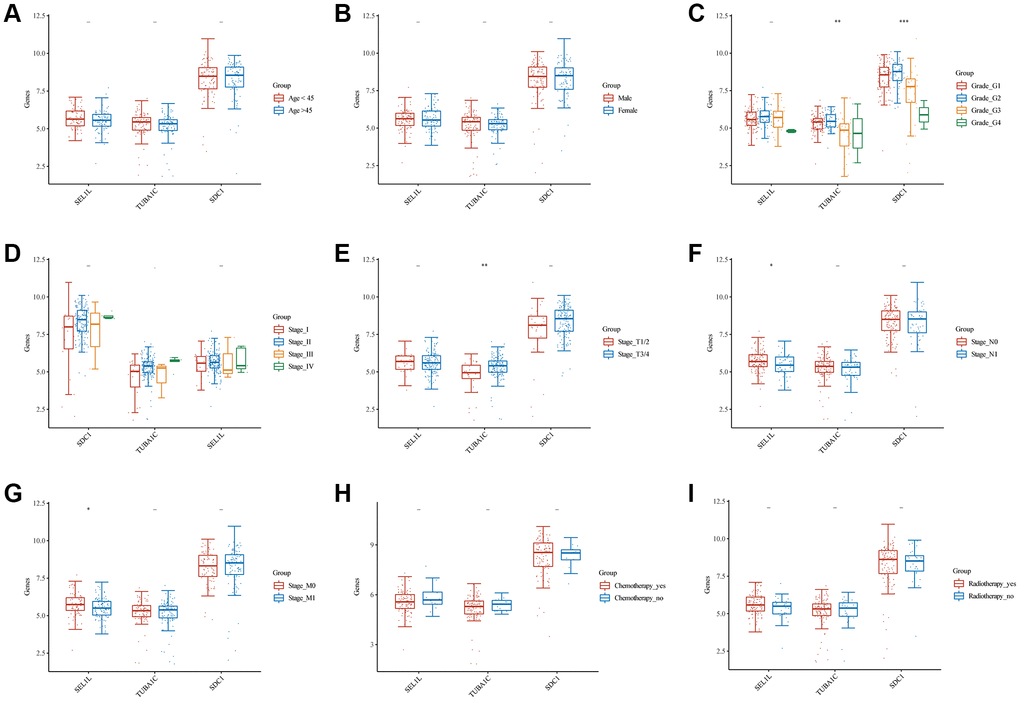
Figure 9. Comparisons of clinical characteristics between 3 GRGs. Age (A), gender (B), clinical grade (C), clinical stage (D), T staging (E), N staging (F), M staging (G), chemotherapy history (H), and radiotherapy history (I) of high and low SEL1L/TUBA1C/SDC1 expression groups.
The biological significance of SEL1L/TUBA1C/SDC1 in pancreatic cancer
TCGA-pancreatic cancer data were classified according to NRG expression levels, SEL1L, TUBA1C, and SDC1, and each group was analyzed using GO and KEGG. The cutoff was set so that the top 50% represented high expression of SDC1, SEL1L, and TUBA1C and the bottom 50% represented low expression of these genes.
High expression of SDC1 in TCGA-pancreatic cancer cohort resulted in 269 upregulated genes and 85 downregulated genes (Figure 10A, 10B). The 269 upregulated genes were associated with pancreatic physiological functions (including epidermal development, keratinocyte differentiation, and ECM organization) and activation processes such as the PI3K-Akt signaling pathway, Wnt signaling pathway, and ECM receptor interaction (Figure 10C, 10D). The 85 downregulated genes were mainly involved in physiological processes, including protein secretion, vitamin metabolic process, and humoral immune response, together with activation processes, such as the PPAR signaling pathway and protein digestion (Figure 10E, 10F).
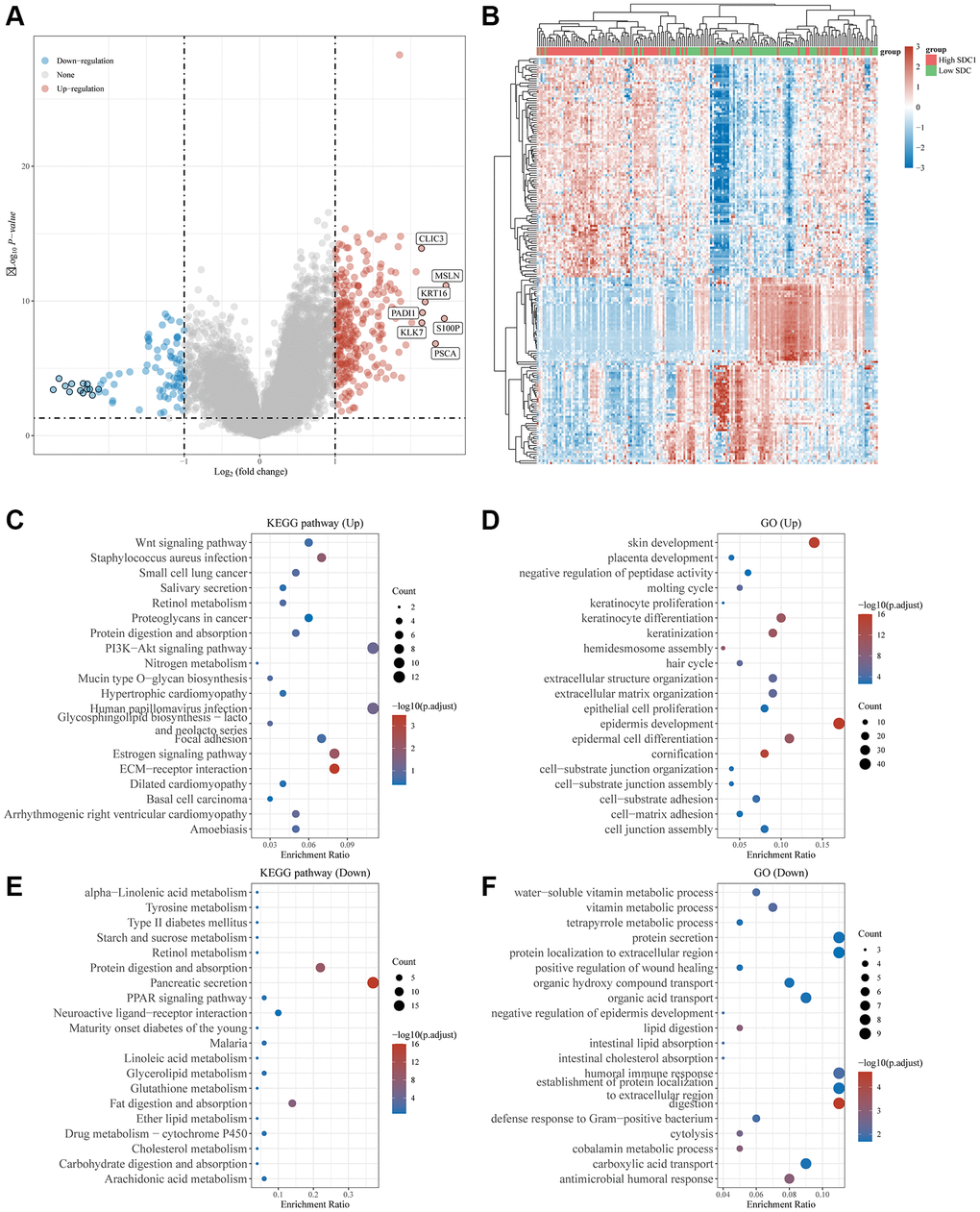
Figure 10. Differential expression and enrichment analysis of high and low SDC1 expression groups. (A) Volcano plots show the differential gene expression between SDC1 high expression and SDC1 low expression groups using fold-change values and adjusted p-values. (B) Heatmap showing differential gene expression (only 50 genes were displayed due to a large number of genes). (C–F) KEGG and GO analyses revealed the signaling pathways associated with up-regulated and down-regulated genes in the SDC1 high/low expressed groups. An enriched pathway is considered when p < 0.05 or FDR <0.05.
High expression of TUBA1C in TCGA-pancreatic cancer cohort included 143 upregulated genes and 42 downregulated genes (Supplementary Figure 3A, 3B). The 143 upregulated genes were associated with pancreatic physiological functions (including epidermal development, keratinocyte differentiation, and ECM organization) and activation processes, such as PI3K-Akt signaling, the estrogen signaling pathway, and ECM receptor interaction (Supplementary Figure 3C, 3D). The 42 downregulated genes were mainly involved in physiological processes, including negative regulation of proteolysis, vitamin metabolic processes, and humoral immune responses (Supplementary Figure 3E, 3F).
High expression of SEL1L in TCGA-pancreatic cancer cohort included 48 upregulated genes and 7 downregulated genes (Supplementary Figure 4A, 4B). The 48 upregulated genes were associated with pancreatic physiological functions (including epidermal development, positive regulation of keratinocyte differentiation, and ECM organization) and activation processes such as pancreatic secretion, protein digestion and absorption, and fat digestion and absorption (Supplementary Figure 4C, 4D).
Correlation between SEL1L/TUBA1C/SDC1 expression, immune status, and stemness
Immune infiltration data from the high- and low-expression SEL1L, TUBA1C, and SDC1 pancreatic cancer groups were gathered using CIBERSORT algorithms. High levels of SDC1 expression positively correlated with naive B cells (p < 0.01), CD8+ T cells (p < 0.001), and monocytes (p < 0.001), and poorly correlated with M0 macrophages (p < 0.001) (Figure 11A). High SEL1L levels positively correlated with M1 macrophages (p < 0.05), M2 macrophages (p < 0.05), resting myeloid dendritic cells (p < 0.01), activated mast cells (p < 0.01), and neutrophils (p < 0.01), and poorly correlated with memory B cells (p < 0.05), follicular helper T cells (p < 0.01), and Tregs (p < 0.001) (Supplementary Figure 5A). High TUBA1C levels positively correlated with M0 macrophages (p < 0.05) and M1 macrophages (p < 0.05), but poorly correlated with naive B cells (p < 0.05) and CD8+ T cells (p < 0.05) (Supplementary Figure 5E).
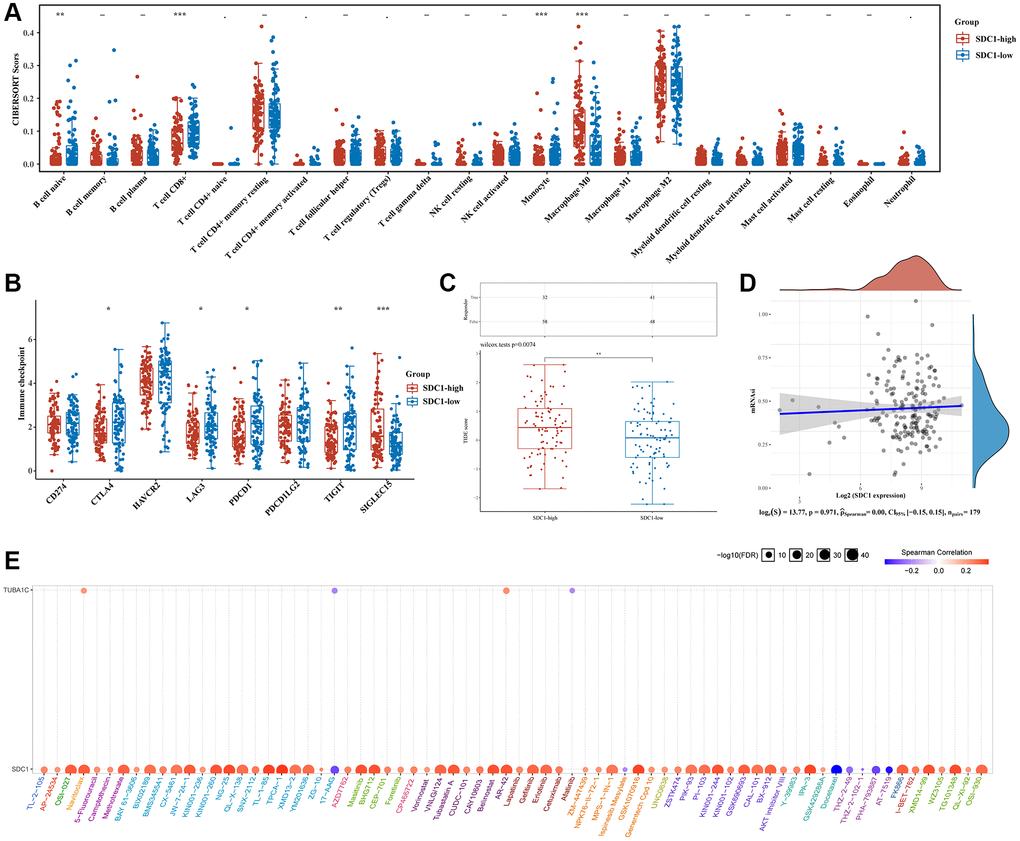
Figure 11. Comparison of immune status and stemness between groups that express high and low levels of SDC1. (A) An analysis of immune infiltration was obtained using the CIBERSORT algorithm for the high expression group of SDC1 and the low expression group of SDC1; the horizontal axis represents immune cells, while the vertical axis displays immune scores (*p < 0.05, **p < 0.01, ***p < 0.001). (B) Comparison of immune-checkpoint gene expression in SDC1 high expression group and SDC1 low expression group. (C) Table showing immune response statistics and immune response scores for different groups. (D) With the OCLR algorithm, SDC1 low expression, and SDC1 high expression groups were compared for stemness. (E) The correlation between SDC1/TUBA1C and GDSC drug sensitivity in PC.
Next, we examined the relationship between ICGs and SEL1L, TUBA1C, and SDC1. SDC1 expression strongly correlated with SIGLEC15 (p < 0.001) and poorly correlated with CTLA4 (p < 0.05), LAG3 (p < 0.05), PDCD1 (p < 0.05), and TIGIT (p < 0.01) (Figure 11B). SEL1L expression positively correlated with three out of eight ICGs including CD274 (p < 0.001), HAVCR2 (p < 0.01), and PDCD1LG2 (p < 0.001) (Supplementary Figure 5B). TUBA1C expression strongly correlated with CD274 (p < 0.05) and SIGLEC15 (p < 0.01) (Supplementary Figure 5F). The TIDE algorithms revealed that high SDC1 expression correlated with a poor immune response (Figure 11C), whereas the expression of SEL1L and TUBA1C was not closely related to the immune response (Supplementary Figure 5C and 5G). There was no crucial correlation between stemness and the expression of SDC1 (Figure 11D), SEL1L (Supplementary Figure 5D), or TUBA1C using the OCLR algorithms (Supplementary Figure 5H).
Drug-sensitivity analysis of SEL1L/TUBA1C/SDC1 in pancreatic cancer
Gene expression-drug correlation analysis is necessary to develop a therapeutic target. Drug-sensitivity analysis showed that the expression of SDC1 and TUBAC1 was positively correlated with some or most medications (Figure 11E). Remarkably, high SDC1 expression was significantly associated with nearly all the existing drugs. This indicated that SDC1 might be a possible therapeutic target for pancreatic cancer.
Validating the expression of SEL1L/TUBA1C/SDC1 in vitro and in vivo
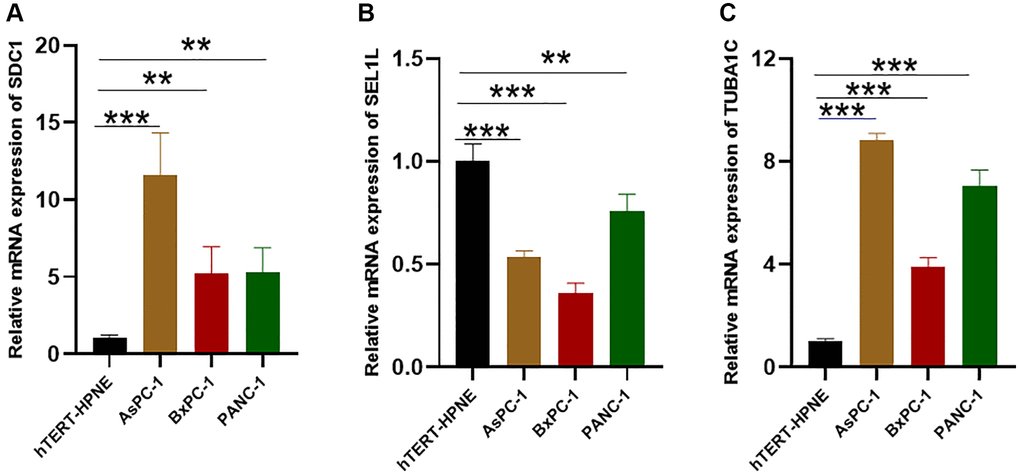
The SEL1L/TUBA1C/SDC1 mRNA expression levels were compared in normal and pancreatic cancer tissues using TCGA. Pancreatic cancer samples had a higher expression of TUBA1C and SDC1 compared with the standard samples, while SEL1L expression was lower in vitro and in vivo (Figure 12A). A comparison of SEL1L/TUBA1C/SDC1 mRNA expression levels in various pancreatic cancer cell lines using the Cancer Cell Line Encyclopedia (CCLE) database showed that most pancreatic cancer cells expressed less SEL1L than SDC1 or TUBA1C (Figure 12B). Additionally, we compared the levels of SEL1L/TUBA1C/SDC1 expression in normal and pancreatic cancer tissues using the Human Protein Atlas (HPA) database. In the HPA database, the expression levels of TUBA1C, SDC1, and SEL1L displayed a comparable pattern (Figure 12C).
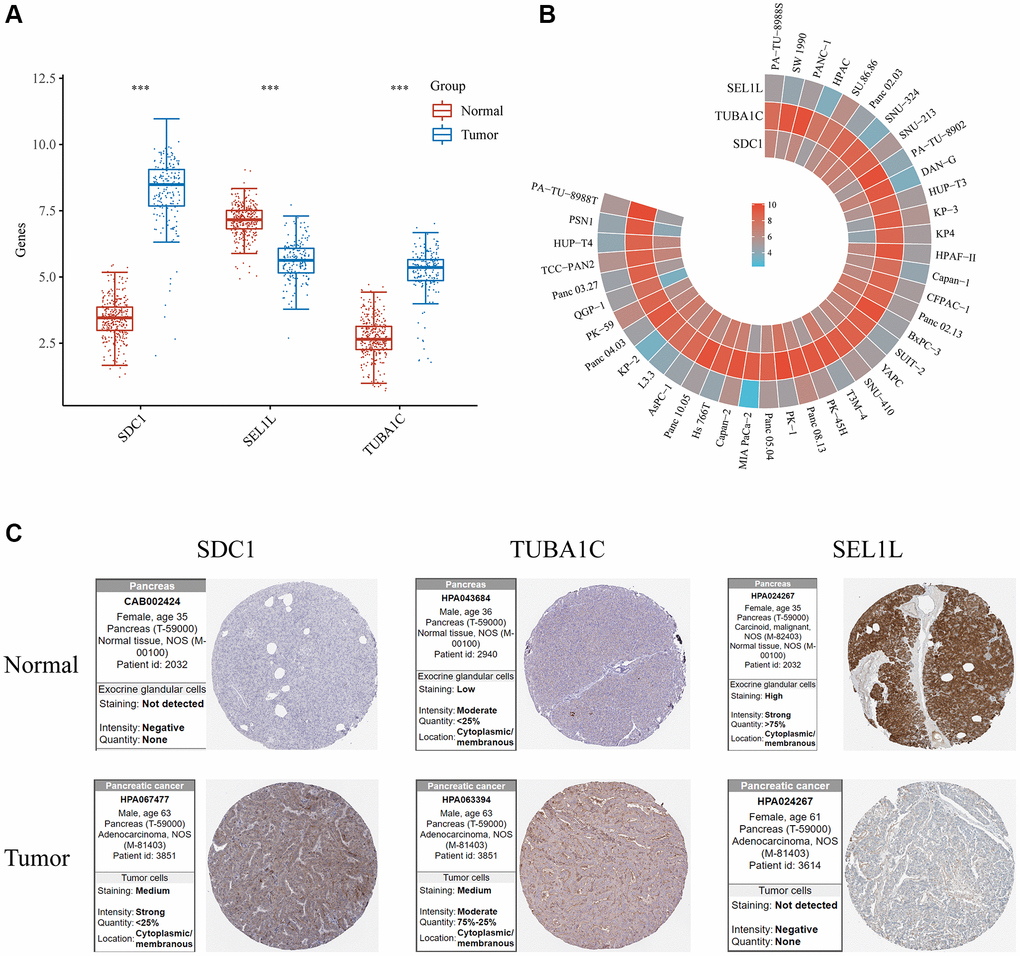
Figure 12. Validation of the mRNA/protein expression levels of SDC1/SEL1L/TUBA1C in vitro and in vivo. (A) The mRNA expression levels of SDC1/SEL1L/TUBA1C of PC and normal pancreas in TCGA database. (B) The mRNA expression levels of SDC1/SEL1L/TUBA1C of PC cell lines in the CCLE database. (C) The protein expression levels of SDC1/SEL1L/TUBA1C of PC and normal pancreas in the HPA database.
Discussion
Protein glycosylation is the most common post-translational modification that serves diverse biological functions [28]. Almost all proteins are glycosylated in at least one way during their synthesis [29]. A new hallmark of cancer is aberrant glycosylation, which plays a critical role in tumor biology [11]. This may offer an opportunity to predict and treat cancer outcomes. Glycosylation-related gene-based signatures predicted the prognosis of ovarian cancer and head and neck squamous cell carcinoma [30, 31]. However, the role of GRGs in pancreatic cancer is poorly studied; therefore, this study determined their correlation.
Precision medicine is a new approach for obtaining and integrating information from biomedical research and clinical practice [32]. The higher success rates of precision medicine in treating HER2-positive breast cancer [33] and EGFR-positive lung cancer [34] highlight its potential to widely change clinical practice. Our study divided samples into four clusters (C1, C2, C3, and C4) based on the DE-GRG dataset of pancreatic cancer, and examined the differences between the clusters. Survival probability was significantly different between these four clusters using Kaplan–Meier plots: C4 and C2 had the worst and best prognosis, respectively. Immune infiltration and ICG analysis of the four groups revealed significant differences in the immune microenvironment. TIDE analysis confirmed differences in immune responses among the four clusters. These findings show that glycosylation is closely associated with pancreatic cancer and highlight its prognostic value.
We identified three GRGs closely related to pancreatic cancer: SEL1L, TUBA1C, and SDC1. Syndecan 1 (SDC1) is a transmembrane heparan sulfate proteoglycan component that has a variety of functions in the development, proliferation, adhesion, and angiogenesis of tumor cells [35, 36]. In general, SDC1 is downregulated in gastrointestinal cancers. Loss of epithelial SDC1 is associated with poor prognosis in hepatocellular carcinoma, colorectal cancer, and gastric cancer patients, together with high tumor volume and high histological grade [37, 38]. Nevertheless, SDC1 levels are solely elevated in pancreatic cancer (the only gastrointestinal malignancy) which speeds up tumor growth [39]. Serum SDC1 is a promising new biomarker for patients with pancreatic cancer [40]. Suppressor Enhancer Lin12 1-like (SEL1L) is a single-transmembrane protein that resides in the ER and destroys misfolded proteins [41–44]. The SEL1L variant genotype rs12435998 contributes to survival time in pancreatic cancer patients who have received combined chemotherapy and pancreaticoduodenectomy [45]. SEL1L expression reduces pancreatic carcinoma cell aggressiveness in vivo and in vitro [46]. Moreover, SEL1 regulates the adhesion and proliferation of β-cells through interaction with β1 integrin signaling [47]. Tubulin Alpha 1c (TUBA1C) is a subtype of α-tubulin that is highly correlated with microtubule structure that is essential for cell division and mitosis [48, 49]. Moreover, TUBA1C plays a vital role in cell cycle signaling pathways [50] and can significantly affect tumor growth and progression [51, 52]. Patients with pancreatic cancer have shorter OS when TUBA1C is overexpressed [53]. The findings of our study on SDC1/TUBAC/SEL1L are consistent with those of previous studies.
We created a three-gene signature that precisely predicts the prognosis of individuals with pancreatic cancer on the basis of these three GRGs using data from TCGA and ICGC cohorts. Both datasets showed that low-risk patients had a superior OS compared to high-risk patients. A recent study predicted the prognosis of pancreatic cancer using a two-gene signature (CASP4 and NLRP1) based on genes related to pyroptosis [25]. Additionally, the usefulness of a three-gene signature (PRKN, SRC and VDAC1) was evaluated based on genes related to mitophagy to predict survival in pancreatic cancer patients [26]. Decision curve analysis revealed that the proposed model provided better clinical benefits. Furthermore, our study developed independent prognostic indicators (age scores and risk scores) and a nomogram to accurately predict 1-, 3-, and 5-year survival rates. This may help improve individualized treatment strategies for patients with pancreatic cancer. These results showed that glycosylation-related signatures were significantly associated with pancreatic cancer patient prognosis and were better predictors of pancreatic cancer outcomes.
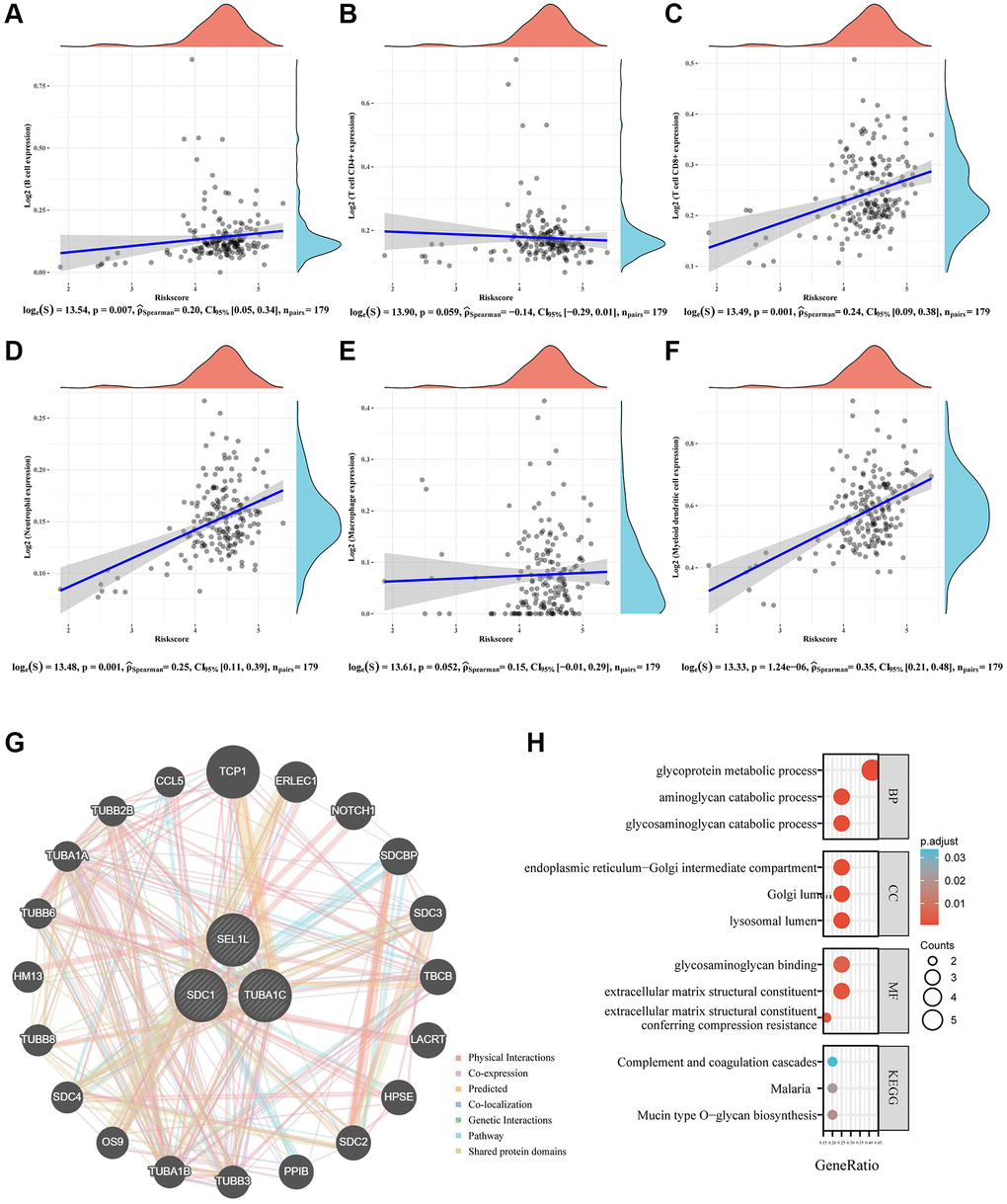
Recent advances in immunotherapy have led to notable improvements in the treatment of a wide variety of cancers [54]. Thus, we looked into the potential effects of signals related to glycosylation in the immunological microenvironment. High-risk patients in TCGA cohort had immunological ratings that were noticeably greater than those of low-risk patients. Higher immune scores are linked to poorer prognosis in patients with pancreatic cancer [55, 56]. Correlations between the signature and the immune landscape indicated that this signature could help predict the number of CD8+ T cells, B cells, neutrophils, and myeloid dendritic cells. This might explain why high-risk patients had a poor prognosis.
Drug-sensitivity analysis using the Genomics of Drug Sensitivity in Cancer (GDSC) database showed that SDC1 expression was closely related to existing drugs. Interestingly, a previous study found that SDC1+ cell lines were susceptible to indatuximab ravtansine in breast cancer [57]. Hepatocellular carcinoma cell lines are platinum-resistant when syndecan-1 (SDC1) is upregulated [58]. Our results indicate that SDC1 may be a therapeutic target for the treatment of pancreatic cancer.
This study had a few limitations. First, it used public datasets without verifying or validating the results using in vitro or in vivo models. Thus, the glycosylation-related signature must be validated in large-scale prospective studies to demonstrate its robustness. Second, our nomogram was not externally validated because of the lack of specific clinical data for ICGC. Furthermore, our results were inconsistent with respect to immune infiltration, tumor stemness, and ICB. Nevertheless, there is no gold standard approach in the growing field of GRGs and their role in cancer. Therefore, we integrated as many analytic strategies and sources as possible to solidify our findings.
In conclusion, our findings indicate that pancreatic cancer and normal tissues express differential GRGs and that pancreatic cancer samples can be divided into four subgroups. We established a prognostic model based on SDC1/TUBAC/SEL1L with favorable prediction performance for pancreatic cancer. The prognostic signature significantly correlated with clinical outcomes, immune infiltration, and pathway enrichment. The findings of this study provide insights into the role of GRGs in the prediction of clinical outcomes in pancreatic cancer.
Materials and Methods
Screening and integrating data
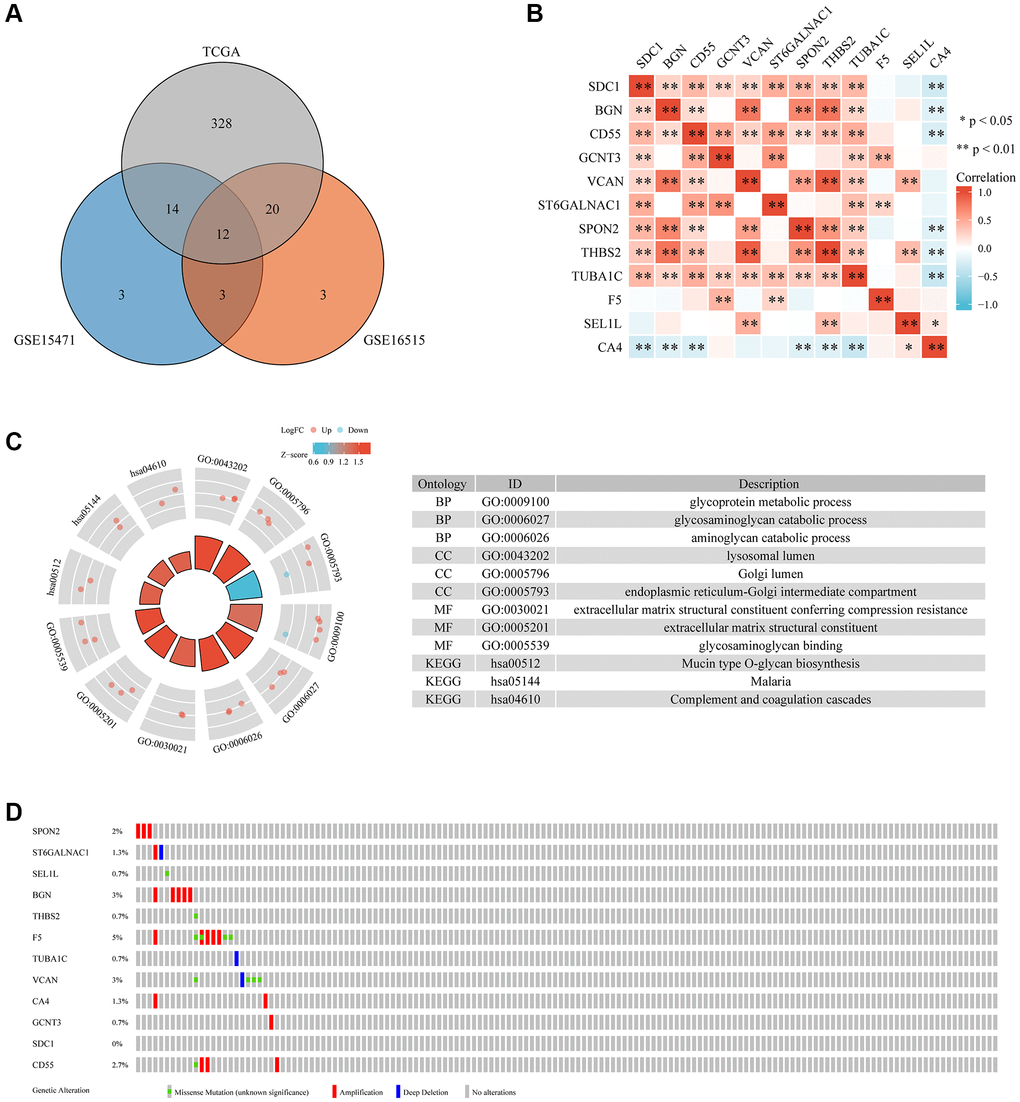
TCGA (https://portal.gdc.cancer.gov/), GEO (https://www.ncbi.nlm.nih.gov/geo/), and the ICGC (https://dcc.icgc.org/) databases were used to obtain transcriptome fragments per kilo base per million mapped reads (FPKM) data and clinical details. The Genotype-Tissue Expression (GTEx) dataset of normal pancreatic samples was obtained from the UCSC Xena website (https://xenabrowser.net/) to investigate differentially expressed genes. Additionally, 636 GRGs were downloaded from the Molecular Signatures Database (MSigDB, http://www.gsea-msigdb.org/gsea/msigdb/). We then extracted GRGs that co-existed in TCGA, GSE16515, and GSE15471 datasets for further analysis. Mutations in GRGs in pancreatic cancer were analyzed using cBioPortal (http://www.cbioportal.org/). Prognostic model construction and validation relied on TCGA, GEO, and ICGC cohort datasets using log2(x + 1) to ensure that gene expression levels were maintained across training and testing. Moreover, GRG mutations in pancreatic cancer were examined using cBioPortal (https://www.cbioportal.org/).
Enrichment analysis
R (version 4.0.5)’s limma package was used to compare DE-GRGs in pancreatic cancer tissues to those in healthy pancreatic tissues. The DE-GRG screening thresholds were set to |logFC| > 1 and p < 0.05. Cluster profiles were used to enrich genes with GO and KEGG to identify potential signaling pathways involved in DE-GRGs. Spearman’s correlation was applied using the R package ggplot2 to detect correlations between DE-GRGs. p < 0.05 were regarded as significant (*p < 0.05).
Consistent clustering of molecular subgroups
A consensus analysis was performed using the Consensus Cluster Plus package of R [59] and a survival analysis to compare the prognostic differences between the subgroups. The PAC structure identifying the default cluster number is repeated 100 times to extract 80% of the sample with clusterAlg = “hc,” and innerLinkage = “ward. D2”. A heatmap (v1.0.12) was used to analyze clustering with R software 4.0.3. Gene expression heat maps were compiled for genes with variance greater than 0.1. The top 25% of genes were extracted and displayed after sequencing according to variance depending on the input target gene number. We compared different subtypes and clinical features using ggplot2 and heatmaps from R (v4.0.3). The threshold for statistical significance was fixed at p < 0.05.
Assessment of immune infiltration, immune checkpoint genes (ICGs), response prediction, and stemness
CIBERSORT (a component of the R software package immunedeconv (https://grst.github.io/immunedeconv)) was used to examine the immune infiltration of various subtypes [22]. The relationship between GRG expression and eight common ICGs was examined (SIGLEC15, TIGIT, CD274, CTLA4, HAVCR2, LAG3, PDCD1, PDCD1LC2, and HAVCR2). Immune checkpoint blockade treatment responses were predicted using the TIDE algorithm (ICB) [22]. The mRNAsi was determined using an OCLR approach [24]. We identified the gene expression profile of 11,774 genes using the mRNA expression signature. Spearman’s correlation analysis was performed on RNA expression data. The minimum value was subtracted from the maximum value, and the result was divided by the maximum value to assign a range of (0,1) to the dryness index. Visualization was accomplished using the R software tools ggplot2 and heatmap (v4.0.3).
Prognostic signature establishment and validation
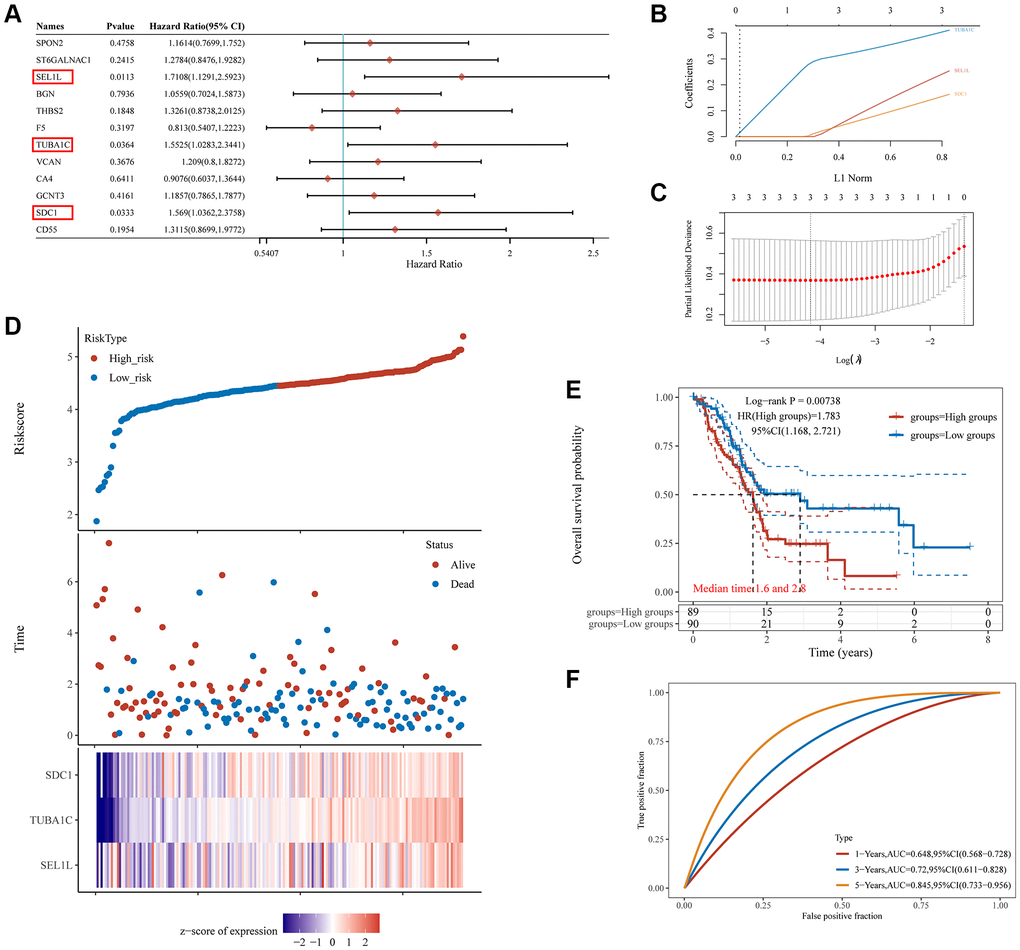
We used the survival R package and the log-rank test to conduct a Kaplan–Meier analysis to determine the prognostic value of the DE-GRGs on overall survival. P < 0.05 were regarded as significant in statistics. A prognostic model was created using LASSO Cox regression analysis of DE-GRGs from the Ggrisk program [60]. A regression coefficient (β) was developed from multivariate Cox regression analysis, and the Prognosis Index (PI) = (βmRNA1 × expression level of mRNA1) + (βmRNA2 × expression level of mRNA2) + … + (βmRNAn × expression level of mRNAn). The patients were divided into low- and high-risk subgroups in accordance with their median risk scores. The prediction power of the prognostic model was evaluated using Kaplan–Meier survival analysis. A time-related ROC analysis was carried out to assess the prognostic capacity of the risk model using the timeROC program.
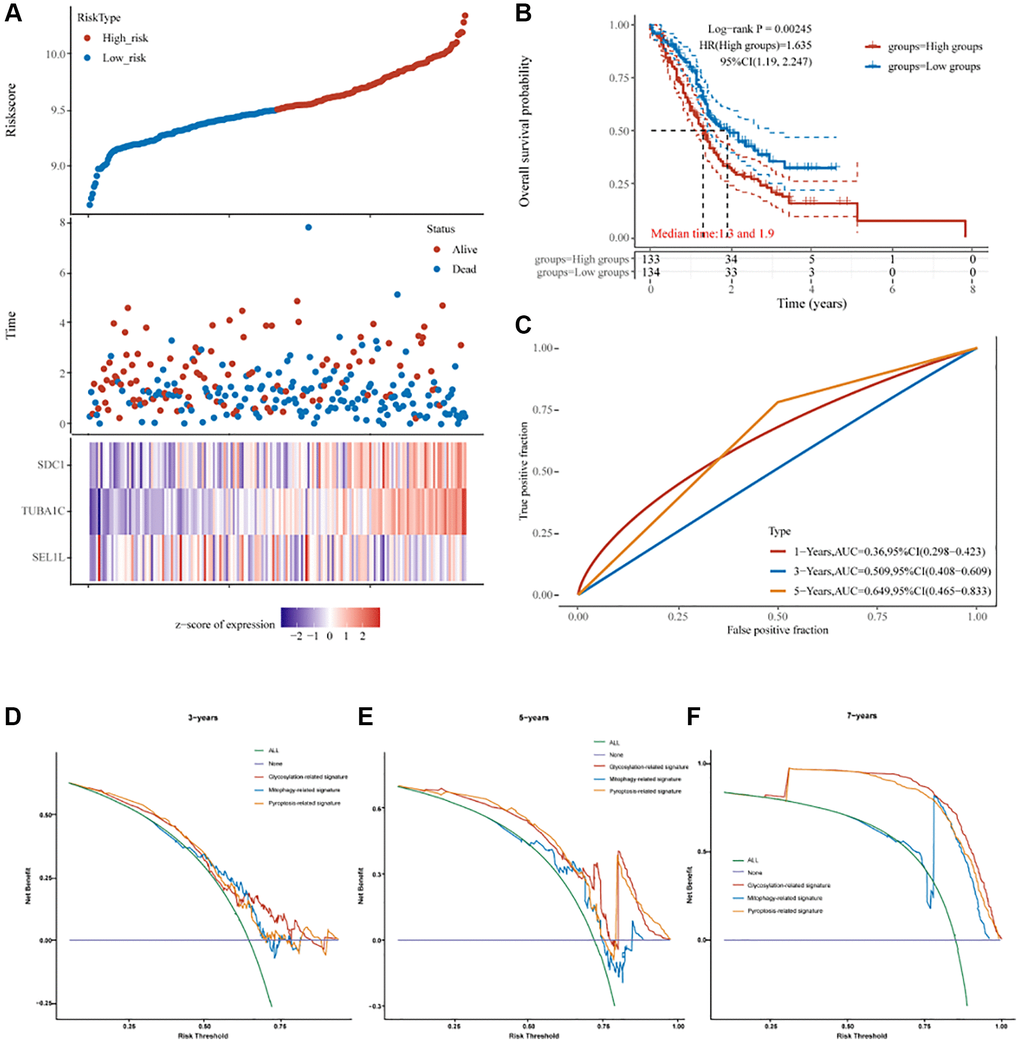
The ICGC database was used to validate the glycosylation-related signature risk-score model. The risk scores were calculated in the same manner, and patients were categorized based on the median risk score. Kaplan–Meier and ROC curve analyses were performed. The clinical benefit of the prognostic signature was assessed using DCA [61].
Developing and evaluating a predictive nomogram
Univariate and multivariate Cox proportional hazards regression analyses were used to determine whether the predictive power of the prognostic model was independent of conventional clinical characteristics. The 1-, 3-, and 5-year survival probabilities of pancreatic cancer were evaluated using an independent prognostic factor nomogram [62]. Calibration plots were used for internal validation to verify their accuracy.
Analysis of drug response and sensitivity in GRGs
Glycosylation-related genes were analyzed using GSCALite for drug sensitivity [63]. Correlations were determined by Spearman’s correlation analysis between mRNA expression levels of GRGs and the 50% inhibitory concentration values for small molecules against various cells in the GDSC database.
Evaluation of GRG expression
The expression of GRGs was evaluated using ggplot2 and the ggdendro package to visualize expression in cells from the CCLE (http://www.broadinstitute.org/ccle) database. HPA (https://www.proteinatlas.org/) provided immunohistochemistry data for clinical samples.
Quantitative real-time PCR (qRT-PCR)
Validation of the mRNA expression levels of SDC1/SEL1L/TUBA1C in PC cell lines (AsPC-1, BxPC-3, PANC-1) and a control cell line (hTERT-HPNE) was done. The PC cell lines were kindly provided by Suzhou Haixing Biosciences Co., Ltd. (Suzhou, China), and the normal pancreatic cell line was obtained from Wuhan Sunncell Biotech Co., Ltd., (Wuhan, China). The PC cell lines and hTERT-HPNE were maintained in RPMI 1640 media with 10% Gibco FBS. All the cells were cultured at 37°C with 5% CO2. Total RNA were isolated from cells using the SPARKeasy bacterial/cell RNA kit (Sparkjade, Shandong, China) and reverse transcription was subsequently performed using the HiScript III RT SuperMix for qPCR (+gDNA wiper) (#R323, Vazyme, China). qRT-PCR was performed with ChamQ Universal SYBR qPCR Master Mix (#Q711, Vazyme) on a QuantStudio™ 1 Plus System (Thermo Fisher Scientific, USA). GAPDH mRNA was employed as a reference gene for normalization of expression, and the 2−ΔΔCt method was applied to quantify changes in the expression of target mRNAs within samples. Primer sequences are listed in Supplementary Table 4. All experiments were repeated at least three times.
Statistical analysis
Log-rank, Chi-square, Wilcoxon, and Kruskal-Wallis tests were used to compare the variables. The threshold for statistical significance was fixed at p < 0.05. R was used to perform all statistical analyses.
Supplementary Materials
Author Contributions
Conceptualization: Huidong Hu, Mingang He. Methodology: Huidong Hu, Mingang He. Formal analysis and software: Mingang He. Supervision: Hengmin Tao, Baosheng Li. Validation: Bingsheng He. Experiments: Bingsheng He. Writing – original draft: Huidong Hu, Mingang He.
Conflicts of Interest
The authors declare no conflicts of interest related to this study.
Ethical Statement
All clinical information and data were obtained from public databases, and therefore, approval from the ethics committee is not required for this study.
Funding
This work was funded by the National Natural Science Foundation of China (No. 81874224), the Academic Promotion Program of Shandong First Medical University (No. 2019LJ004), the Taishan Scholar Construction Project (No. ts20120505), and the Tumor Prevention and Control Joint Fund of Shandong Province Natural Science Fund, China (No. ZR2019LZL008).
References
- 1. Sodir NM, Kortlever RM, Barthet VJA, Campos T, Pellegrinet L, Kupczak S, Anastasiou P, Swigart LB, Soucek L, Arends MJ, Littlewood TD, Evan GI. MYC Instructs and Maintains Pancreatic Adenocarcinoma Phenotype. Cancer Discov. 2020; 10:588–607. https://doi.org/10.1158/2159-8290.CD-19-0435 [PubMed]
- 2. Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer Statistics, 2021. CA Cancer J Clin. 2021; 71:7–33. https://doi.org/10.3322/caac.21654 [PubMed]
- 3. Van Cutsem E, Hidalgo M, Canon JL, Macarulla T, Bazin I, Poddubskaya E, Manojlovic N, Radenkovic D, Verslype C, Raymond E, Cubillo A, Schueler A, Zhao C, Hammel P. Phase I/II trial of pimasertib plus gemcitabine in patients with metastatic pancreatic cancer. Int J Cancer. 2018; 143:2053–64. https://doi.org/10.1002/ijc.31603 [PubMed]
- 4. Peng W, Zhao J, Dong X, Banazadeh A, Huang Y, Hussien A, Mechref Y. Clinical application of quantitative glycomics. Expert Rev Proteomics. 2018; 15:1007–31. https://doi.org/10.1080/14789450.2018.1543594 [PubMed]
- 5. Yu A, Zhao J, Peng W, Banazadeh A, Williamson SD, Goli M, Huang Y, Mechref Y. Advances in mass spectrometry-based glycoproteomics. Electrophoresis. 2018; 39:3104–22. https://doi.org/10.1002/elps.201800272 [PubMed]
- 6. Varki A. Biological roles of glycans. Glycobiology. 2017; 27:3–49. https://doi.org/10.1093/glycob/cww086 [PubMed]
- 7. Kailemia MJ, Xu G, Wong M, Li Q, Goonatilleke E, Leon F, Lebrilla CB. Recent Advances in the Mass Spectrometry Methods for Glycomics and Cancer. Anal Chem. 2018; 90:208–24. https://doi.org/10.1021/acs.analchem.7b04202 [PubMed]
- 8. Breitling J, Aebi M. N-linked protein glycosylation in the endoplasmic reticulum. Cold Spring Harb Perspect Biol. 2013; 5:a013359. https://doi.org/10.1101/cshperspect.a013359 [PubMed]
- 9. Mescher MF, Strominger JL. Purification and characterization of a prokaryotic glycoprotein from the cell envelope of Halobacterium salinarium. J Biol Chem. 1976; 251:2005–14. [PubMed]
- 10. Munkley J. The glycosylation landscape of pancreatic cancer. Oncol Lett. 2019; 17:2569–75. https://doi.org/10.3892/ol.2019.9885 [PubMed]
- 11. Munkley J, Elliott DJ. Hallmarks of glycosylation in cancer. Oncotarget. 2016; 7:35478–89. https://doi.org/10.18632/oncotarget.8155 [PubMed]
- 12. Reis CA, Osorio H, Silva L, Gomes C, David L. Alterations in glycosylation as biomarkers for cancer detection. J Clin Pathol. 2010; 63:322–9. https://doi.org/10.1136/jcp.2009.071035 [PubMed]
- 13. Drake RR. Glycosylation and cancer: moving glycomics to the forefront. Adv Cancer Res. 2015; 126:1–10. https://doi.org/10.1016/bs.acr.2014.12.002 [PubMed]
- 14. Chandler KB, Costello CE, Rahimi N. Glycosylation in the Tumor Microenvironment: Implications for Tumor Angiogenesis and Metastasis. Cells. 2019; 8:544. https://doi.org/10.3390/cells8060544 [PubMed]
- 15. Gupta R, Leon F, Rauth S, Batra SK, Ponnusamy MP. A Systematic Review on the Implications of O-linked Glycan Branching and Truncating Enzymes on Cancer Progression and Metastasis. Cells. 2020; 9:446. https://doi.org/10.3390/cells9020446 [PubMed]
- 16. RodrÍguez E, Schetters STT, van Kooyk Y. The tumour glyco-code as a novel immune checkpoint for immunotherapy. Nat Rev Immunol. 2018; 18:204–11. https://doi.org/10.1038/nri.2018.3 [PubMed]
- 17. Qorri B, Harless W, Szewczuk MR. Novel Molecular Mechanism of Aspirin and Celecoxib Targeting Mammalian Neuraminidase-1 Impedes Epidermal Growth Factor Receptor Signaling Axis and Induces Apoptosis in Pancreatic Cancer Cells. Drug Des Devel Ther. 2020; 14:4149–67. https://doi.org/10.2147/DDDT.S264122 [PubMed]
- 18. Lumibao JC, Tremblay JR, Hsu J, Engle DD. Altered glycosylation in pancreatic cancer and beyond. J Exp Med. 2022; 219:e20211505. https://doi.org/10.1084/jem.20211505 [PubMed]
- 19. Xu L, Pan J, Ding Y, Pan H. Survival-Associated Alternative Splicing Events and Prognostic Signatures in Pancreatic Cancer. Front Genet. 2020; 11:522383. https://doi.org/10.3389/fgene.2020.522383 [PubMed]
- 20. Geng Y, Guan R, Hong W, Huang B, Liu P, Guo X, Hu S, Yu M, Hou B. Identification of m6A-related genes and m6A RNA methylation regulators in pancreatic cancer and their association with survival. Ann Transl Med. 2020; 8:387. https://doi.org/10.21037/atm.2020.03.98 [PubMed]
- 21. Strumillo MJ, Oplová M, Viéitez C, Ochoa D, Shahraz M, Busby BP, Sopko R, Studer RA, Perrimon N, Panse VG, Beltrao P. Conserved phosphorylation hotspots in eukaryotic protein domain families. Nat Commun. 2019; 10:1977. https://doi.org/10.1038/s41467-019-09952-x [PubMed]
- 22. Sturm G, Finotello F, Petitprez F, Zhang JD, Baumbach J, Fridman WH, List M, Aneichyk T. Comprehensive evaluation of transcriptome-based cell-type quantification methods for immuno-oncology. Bioinformatics. 2019; 35:i436–45. https://doi.org/10.1093/bioinformatics/btz363 [PubMed]
- 23. Newman AM, Liu CL, Green MR, Gentles AJ, Feng W, Xu Y, Hoang CD, Diehn M, Alizadeh AA. Robust enumeration of cell subsets from tissue expression profiles. Nat Methods. 2015; 12:453–7. https://doi.org/10.1038/nmeth.3337 [PubMed]
- 24. Malta TM, Sokolov A, Gentles AJ, Burzykowski T, Poisson L, Weinstein JN, Kamińska B, Huelsken J, Omberg L, Gevaert O, Colaprico A, Czerwińska P, Mazurek S, et al, and Cancer Genome Atlas Research Network. Machine Learning Identifies Stemness Features Associated with Oncogenic Dedifferentiation. Cell. 2018; 173:338–54.e15. https://doi.org/10.1016/j.cell.2018.03.034 [PubMed]
- 25. Song W, Liu Z, Wang K, Tan K, Zhao A, Li X, Yuan Y, Yang Z. Pyroptosis-related genes regulate proliferation and invasion of pancreatic cancer and serve as the prognostic signature for modeling patient survival. Discov Oncol. 2022; 13:39. https://doi.org/10.1007/s12672-022-00495-0 [PubMed]
- 26. Zhuo Z, Lin H, Liang J, Ma P, Li J, Huang L, Chen L, Yang H, Bai Y, Sha W. Mitophagy-Related Gene Signature for Prediction Prognosis, Immune Scenery, Mutation, and Chemotherapy Response in Pancreatic Cancer. Front Cell Dev Biol. 2022; 9:802528. https://doi.org/10.3389/fcell.2021.802528 [PubMed]
- 27. Galuppini F, Dal Pozzo CA, Deckert J, Loupakis F, Fassan M, Baffa R. Tumor mutation burden: from comprehensive mutational screening to the clinic. Cancer Cell Int. 2019; 19:209. https://doi.org/10.1186/s12935-019-0929-4 [PubMed]
- 28. Pinho SS, Reis CA. Glycosylation in cancer: mechanisms and clinical implications. Nat Rev Cancer. 2015; 15:540–55. https://doi.org/10.1038/nrc3982 [PubMed]
- 29. Schjoldager KT, Narimatsu Y, Joshi HJ, Clausen H. Global view of human protein glycosylation pathways and functions. Nat Rev Mol Cell Biol. 2020; 21:729–49. https://doi.org/10.1038/s41580-020-00294-x [PubMed]
- 30. Zhao C, Xiong K, Zhao F, Adam A, Li X. Glycosylation-Related Genes Predict the Prognosis and Immune Fraction of Ovarian Cancer Patients Based on Weighted Gene Coexpression Network Analysis (WGCNA) and Machine Learning. Oxid Med Cell Longev. 2022; 2022:3665617. https://doi.org/10.1155/2022/3665617 [PubMed]
- 31. Chen L, Ling Y, Yang H. Comprehensive Analysis of the Potential Prognostic Value of 11 Glycosylation-Related Genes in Head and Neck Squamous Cell Carcinoma and Their Correlation with PD-L1 Expression and Immune Infiltration. J Oncol. 2022; 2022:2786680. https://doi.org/10.1155/2022/2786680 [PubMed]
- 32. Hawgood S, Hook-Barnard IG, O'Brien TC, Yamamoto KR. Precision medicine: Beyond the inflection point. Sci Transl Med. 2015; 7:300ps17. https://doi.org/10.1126/scitranslmed.aaa9970 [PubMed]
- 33. Moasser MM, Krop IE. The Evolving Landscape of HER2 Targeting in Breast Cancer. JAMA Oncol. 2015; 1:1154–61. https://doi.org/10.1001/jamaoncol.2015.2286 [PubMed]
- 34. Maemondo M, Inoue A, Kobayashi K, Sugawara S, Oizumi S, Isobe H, Gemma A, Harada M, Yoshizawa H, Kinoshita I, Fujita Y, Okinaga S, Hirano H, et al, and North-East Japan Study Group. Gefitinib or chemotherapy for non-small-cell lung cancer with mutated EGFR. N Engl J Med. 2010; 362:2380–8. https://doi.org/10.1056/NEJMoa0909530 [PubMed]
- 35. Teng YH, Aquino RS, Park PW. Molecular functions of syndecan-1 in disease. Matrix Biol. 2012; 31:3–16. https://doi.org/10.1016/j.matbio.2011.10.001 [PubMed]
- 36. Czarnowski D. Syndecans in cancer: A review of function, expression, prognostic value, and therapeutic significance. Cancer Treat Res Commun. 2021; 27:100312. https://doi.org/10.1016/j.ctarc.2021.100312 [PubMed]
- 37. Harada K, Masuda S, Hirano M, Nakanuma Y. Reduced expression of syndecan-1 correlates with histologic dedifferentiation, lymph node metastasis, and poor prognosis in intrahepatic cholangiocarcinoma. Hum Pathol. 2003; 34:857–63. https://doi.org/10.1016/s0046-8177(03)00336-8 [PubMed]
- 38. Hashimoto Y, Skacel M, Adams JC. Association of loss of epithelial syndecan-1 with stage and local metastasis of colorectal adenocarcinomas: an immunohistochemical study of clinically annotated tumors. BMC Cancer. 2008; 8:185. https://doi.org/10.1186/1471-2407-8-185 [PubMed]
- 39. Conejo JR, Kleeff J, Koliopanos A, Matsuda K, Zhu ZW, Goecke H, Bicheng N, Zimmermann A, Korc M, Friess H, Büchler MW. Syndecan-1 expression is up-regulated in pancreatic but not in other gastrointestinal cancers. Int J Cancer. 2000; 88:12–20. https://doi.org/10.1002/1097-0215(20001001)88:1%3c12::aid-ijc3%3e3.0.co;2-t [PubMed]
- 40. Yablecovitch D, Ben-Horin S, Picard O, Yavzori M, Fudim E, Nadler M, Levy I, Sakhnini E, Lang A, Engel T, Lahav M, Saker T, Neuman S, et al. Serum Syndecan-1: A Novel Biomarker for Pancreatic Ductal Adenocarcinoma. Clin Transl Gastroenterol. 2022; 13:e00473. https://doi.org/10.14309/ctg.0000000000000473 [PubMed]
- 41. Hampton RY, Gardner RG, Rine J. Role of 26S proteasome and HRD genes in the degradation of 3-hydroxy-3-methylglutaryl-CoA reductase, an integral endoplasmic reticulum membrane protein. Mol Biol Cell. 1996; 7:2029–44. https://doi.org/10.1091/mbc.7.12.2029 [PubMed]
- 42. Gardner RG, Swarbrick GM, Bays NW, Cronin SR, Wilhovsky S, Seelig L, Kim C, Hampton RY. Endoplasmic reticulum degradation requires lumen to cytosol signaling. Transmembrane control of Hrd1p by Hrd3p. J Cell Biol. 2000; 151:69–82. https://doi.org/10.1083/jcb.151.1.69 [PubMed]
- 43. Mueller B, Lilley BN, Ploegh HL. SEL1L, the homologue of yeast Hrd3p, is involved in protein dislocation from the mammalian ER. J Cell Biol. 2006; 175:261–70. https://doi.org/10.1083/jcb.200605196 [PubMed]
- 44. Mueller B, Klemm EJ, Spooner E, Claessen JH, Ploegh HL. SEL1L nucleates a protein complex required for dislocation of misfolded glycoproteins. Proc Natl Acad Sci U S A. 2008; 105:12325–30. https://doi.org/10.1073/pnas.0805371105 [PubMed]
- 45. Liu Q, Chen J, Mai B, Amos C, Killary AM, Sen S, Wei C, Frazier ML. A single-nucleotide polymorphism in tumor suppressor gene SEL1L as a predictive and prognostic marker for pancreatic ductal adenocarcinoma in Caucasians. Mol Carcinog. 2012; 51:433–8. https://doi.org/10.1002/mc.20808 [PubMed]
- 46. Cattaneo M, Orlandini S, Beghelli S, Moore PS, Sorio C, Bonora A, Bassi C, Talamini G, Zamboni G, Orlandi R, Ménard S, Bernardi LR, Biunno I, Scarpa A. SEL1L expression in pancreatic adenocarcinoma parallels SMAD4 expression and delays tumor growth in vitro and in vivo. Oncogene. 2003; 22:6359–68. https://doi.org/10.1038/sj.onc.1206665 [PubMed]
- 47. Diaferia GR, Cirulli V, Biunno I. SEL1L regulates adhesion, proliferation and secretion of insulin by affecting integrin signaling. PLoS One. 2013; 8:e79458. https://doi.org/10.1371/journal.pone.0079458 [PubMed]
- 48. Gilbertson-White S, Perkhounkova Y, Saeidzadeh S, Hein M, Dahl R, Simons-Burnett A. Understanding Symptom Burden in Patients With Advanced Cancer Living in Rural Areas. Oncol Nurs Forum. 2019; 46:428–41. https://doi.org/10.1188/19.ONF.428-441 [PubMed]
- 49. Jordan MA, Wilson L. Microtubules as a target for anticancer drugs. Nat Rev Cancer. 2004; 4:253–65. https://doi.org/10.1038/nrc1317 [PubMed]
- 50. Wang J, Chen W, Wei W, Lou J. Oncogene TUBA1C promotes migration and proliferation in hepatocellular carcinoma and predicts a poor prognosis. Oncotarget. 2017; 8:96215–24. https://doi.org/10.18632/oncotarget.21894 [PubMed]
- 51. Nami B, Wang Z. Genetics and Expression Profile of the Tubulin Gene Superfamily in Breast Cancer Subtypes and Its Relation to Taxane Resistance. Cancers (Basel). 2018; 10:274. https://doi.org/10.3390/cancers10080274 [PubMed]
- 52. Li H, Jiang X, Zhu S, Sui L. Identification of personalized dysregulated pathways in hepatocellular carcinoma. Pathol Res Pract. 2017; 213:327–32. https://doi.org/10.1016/j.prp.2017.01.015 [PubMed]
- 53. Albahde MAH, Zhang P, Zhang Q, Li G, Wang W. Upregulated Expression of TUBA1C Predicts Poor Prognosis and Promotes Oncogenesis in Pancreatic Ductal Adenocarcinoma via Regulating the Cell Cycle. Front Oncol. 2020; 10:49. https://doi.org/10.3389/fonc.2020.00049 [PubMed]
- 54. Shin C, Kim SS, Jo YH. Extending traditional antibody therapies: Novel discoveries in immunotherapy and clinical applications. Mol Ther Oncolytics. 2021; 22:166–79. https://doi.org/10.1016/j.omto.2021.08.005 [PubMed]
- 55. Li L, Deng Z, Xiao Z, Zou W, Liu R. Analysis of Pyroptosis-Related Signature for Predicting Prognosis and Tumor Immune Microenvironment in Pancreatic Cancer. Front Oncol. 2022; 12:770005. https://doi.org/10.3389/fonc.2022.770005 [PubMed]
- 56. Chen H, Zu F, Zeng T, Chen Z, Wei J, Liu P, Li Z, Zhou L, Wang H, Tan H, Tan X. Prognostic Value and Correlation With Tumor Immune Infiltration of a Novel Metabolism-Related Gene Signature in Pancreatic Cancer. Front Oncol. 2022; 11:757791. https://doi.org/10.3389/fonc.2021.757791 [PubMed]
- 57. Schönfeld K, Herbener P, Zuber C, Häder T, Bernöster K, Uherek C, Schüttrumpf J. Activity of Indatuximab Ravtansine against Triple-Negative Breast Cancer in Preclinical Tumor Models. Pharm Res. 2018; 35:118. https://doi.org/10.1007/s11095-018-2400-y [PubMed]
- 58. Yu L, Xu H, Zhang S, Chen J, Yu Z. SDC1 promotes cisplatin resistance in hepatic carcinoma cells via PI3K-AKT pathway. Hum Cell. 2020; 33:721–9. https://doi.org/10.1007/s13577-020-00362-6 [PubMed]
- 59. Wilkerson MD, Hayes DN. ConsensusClusterPlus: a class discovery tool with confidence assessments and item tracking. Bioinformatics. 2010; 26:1572–3. https://doi.org/10.1093/bioinformatics/btq170 [PubMed]
- 60. Tibshirani R. The lasso method for variable selection in the Cox model. Stat Med. 1997; 16:385–95. https://doi.org/10.1002/(sici)1097-0258(19970228)16:4%3c385::aid-sim380%3e3.0.co;2-3 [PubMed]
- 61. Vickers AJ, Cronin AM, Elkin EB, Gonen M. Extensions to decision curve analysis, a novel method for evaluating diagnostic tests, prediction models and molecular markers. BMC Med Inform Decis Mak. 2008; 8:53. https://doi.org/10.1186/1472-6947-8-53 [PubMed]
- 62. Iasonos A, Schrag D, Raj GV, Panageas KS. How to build and interpret a nomogram for cancer prognosis. J Clin Oncol. 2008; 26:1364–70. https://doi.org/10.1200/JCO.2007.12.9791 [PubMed]
- 63. Liu CJ, Hu FF, Xia MX, Han L, Zhang Q, Guo AY. GSCALite: a web server for gene set cancer analysis. Bioinformatics. 2018; 34:3771–2. https://doi.org/10.1093/bioinformatics/bty411 [PubMed]