Introduction
Age related macular degeneration (AMD) is one of the leading cause of visual impairment in developed countries [1,2]. AMD has been classified in two major clinical patterns: the “dry” form which is associated with an atrophic evolution and a slow visual decline and the “neovascular” form which is characterized by choroidal neovascularization (cnv) associated with a rapid and abrupt visual loss [3,4].
AMD is the result of a complex interaction between environmental factors and genetic. Smoking is the most consistently identified modifiable risk factor, but dietary factors, solar insolation, and season of birth may also affect AMD incidence and progression [5,6]. The pathogenesis of neovascular AMD has long been debated but at present it remains not fully elucidated. It encompasses the presence of an inflammatory network involving the macula and the active role of pro-angiogenic factors which lead to choroidal neovascularization and visual loss [7].
Among the various pro-angiogenic factors, vascular endothelial growth factor (VEGF) seems to play a pivotal role in neovascular AMD, and actually anti-VEGF drugs are the only approved therapeutic approach for the treatment of the disease [8–11]. Nevertheless, in addition to VEGF several humoral mediators including fibroblast growth factor, platelet-derived growth factor, interleukin-6 (IL-6), interleukin-8 (IL-8), monocyte chemoattractant protein-1, and insulin-like growth factor-1 (IGF-1) are altered in patients affected by neovascular AMD [12–15].
IGF-1, also called somatomedin C, is a protein that is mainly secreted by the liver as a result of stimulation by growth hormone. IGF-1 is important for both the regulation of normal physiology, as well as a number of pathological states, including cancer [16]. High IGF-1 levels were associated with increased all cause mortality, human studies support the notion that attenuation of GH/IGF-1 signaling may protect from age-related diseases and functional decline [17].
In eyes affected by neovascular AMD, IGF-1 is increased in ocular fluid. Furthermore IGF-1 receptors are expressed in retinal pigmented epithelium cells which are involved in neovascular AMD [18].
To date, only one study investigated systemic IGF-1 concentration in neovascular AMD patients, showing an increment in circulating IGF-1 levels in comparison to healthy controls. The authors demonstrated that early endothelial cells are increased in neovascular AMD and may contribute to IGF-1 elevation [19].
However, in this study only patients with neovascular AMD were included, whereas patients with less advanced stages of AMD were not evaluated. Therefore, it remains unclear if IGF-1 elevation is a consequence of neovascular development in AMD patients, or if IGF-1 is primary involved in the pathogenesis of AMD, as in others aging related diseases, being a causal factor instead of the effect of AMD.
The present study was therefore designed to evaluate the circulating IGF-1 levels in early, intermediate, and neovascular AMD patients in comparison to healthy matched controls.
Results
Overall 224 subjects met the study inclusion criteria and were included in the study, 56 patients in neovascular AMD group (32 type 1 cnv, 18 type 2 cnv, 6 type 3 cnv) (mean age 74±8 years), 56 patients in intermediate AMD group (mean age 73±8 years), 56 patients in early AMD group (mean age 74±1 years), and 56 patients in no AMD group (mean age 73±4 years). Mean best corrected visual acuity (BCVA) and intraocular pressure in four groups are reported in Table 1. For each group 28 male patients and 28 female patients were enrolled.
Table 1. Mean ± standard deviations (SD) Best Corrected Visual Acuity and Intraocular Pressure values detected in four groups.
| Neovascular AMD (n=56) | Intermediate AMD (n=56) | Early AMD (n=56) | No AMD (n=56) | P (ANOVA) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| BCVA | logMAR | 0.58±0.06 * | 0.09±0.05 * | 0.04±0.05 ° | 0.01±0.02 | <0.001 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Intraocular pressure | mmHg | 14.2±2.6 | 14.6±2.5 | 14.3±2.1 | 14.4±2.5 | 0.787 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| BCVA: Best Corrected Visual Acuity | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Tukey HSD vs no AMD: * p<0.001, ° p=0.007 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Mean IGF-1 values in all patients
As shown in Table 2 the overall mean ± standard deviations (SD) IGF-1 values was significantly different between groups (P<0.001, ANOVA). Compared with the no AMD group, the mean IGF-1 values was significantly higher in the neovascular AMD group (Tukey HSD p<0.001) and in the intermediate AMD group (Tukey HSD p=0.002); no significant difference between early AMD group and no AMD group (Tukey HSD p =0.911), Figure 1.
Table 2. Mean ± standard deviations (SD) IGF-1 values detected in four groups.
| Neovascular AMD (n=56) | Intermediate AMD (n=56) | Early AMD (n=56) | No AMD (n=56) | P (ANOVA) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Overall | 146±40 * | 127±29 ° | 107±32 | 103±36 | <0.001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Males | 169±34 * | 143±30 ¨ | 118±35 | 114±38 | <0.001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Females | 123±32 * | 111±16 § | 97±25 | 92±30 | <0.001 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Tukey HSD vs no AMD: * p<0.001, ° p=0.002, ¨ p=0.011, § p=0.038 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
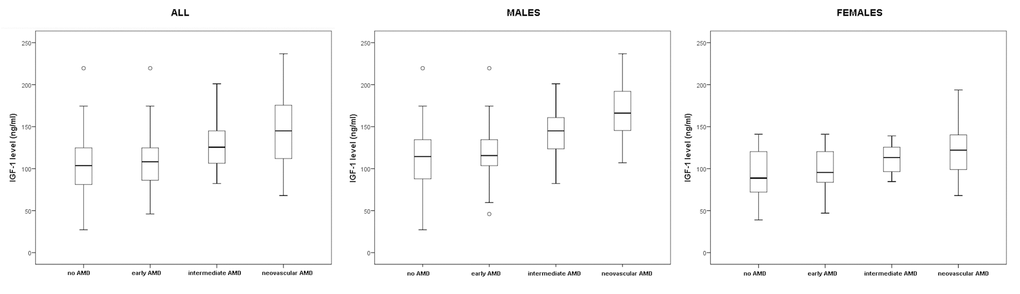
Figure 1. IGF-1 levels in all patients, males and females, in four groups.
Mean IGF-1 values in male patients
The overall mean ± (SD) IGF-1 values in male patients was significantly different between groups (P<0.001, ANOVA). Compared with the no AMD group, the mean ± (SD) IGF-1 values was significantly higher in the neovascular AMD group (Tukey HSD p<0.001) and in the intermediate AMD group (Tukey HSD p=0.011); no difference was seen with early AMD group (Tukey HSD p =0.975).
Mean IGF-1 values in female patients
The overall mean ± (SD) IGF-1 values was significantly different between groups (P<0.001, ANOVA). Compared with the no AMD group, the mean ± (SD) IGF-1 values was significantly higher in the neovascular AMD group (Tukey HSD p<0.001) and in the intermediate AMD group (Tukey HSD p=0.038), but not in early AMD group (Tukey HSD p =0.905).
Correlation between IGF-1 and age
A significant correlation was found between mean IGF-1 values and age in early AMD group (r=-0. 342, p=0.010) and no AMD group (r=-0.317, p=0.017), but no significant in neovascular AMD group (r=-0.117, p=0.389) and intermediate AMD (r=-0. 211, p=0.118), Figure 2.
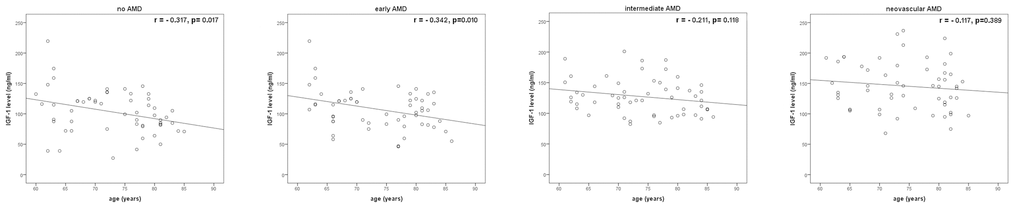
Figure 2. Correlations between IGF-1 levels and age in four groups.
Discussion
AMD is a retinal degenerative disorder characterized by complex and not entirely understood pathogenesis. Several cytokines that promote retinal inflammation and angiogenesis has been suggested to be involved. Among these, there are clinical and experimental evidences on the role of retinal IGF-1 as a mediator of retinal inflammation and neovascular formation [20,21]. To address this hypothesis, we evaluated circulating IGF-1 levels in patients with various stages of AMD. Our results indicate that serum levels of IGF-1 are higher in intermediate and neovascular AMD patients in comparison with early and no AMD patients.
Dong Min Cha and associates [18] demonstrated the presence of higher levels of various cytokines, chemokines and growth factors, including IGF-1, in the aqueous humor samples of patients affected by AMD in comparison with control subjects.
In a previous study Machalinska and associates demonstrated higher IGF-1 plasma concentration of IGF-1 in patients with neovascular AMD in comparison to healthy subjects. Furthermore in their study the authors also reported an association of higher IGF-1 levels with an increase of early endothelial progenitor cells. Albeit the latter association does not prove a cause to effect relationship, the authors hypothesized that angiogenesis under hypoxic conditions may represent the trigger that may explain the above mentioned observations [19]. They also suggested as a possible explanation a disturbed local synthesis of the cytokines and growth factors under conditions of chronic vascular endothelial injury. It should be kept in mind that IGF-1 is a well-known retinal pro-angiogenic cytokine, and it has been demonstrated that IGF-1 induces retinal neovascularization in animal models [22]. This may be of particular relevance under condition of long-term chronic hypoxia, in contrast to VEGF which may be more readily increased in the early phases of retinal ischemia.
In agreement with the study of Machalinska, our results showed an increase in IGF-1 values in patients with neovascular AMD compared to healthy patients. However, a novel contribution of our present study is the observation of a significant increase in IGF-1 levels also in patients with intermediate stages of the disease. These data suggest that IGF-1 may be already elevated in stages of the retinal degeneration prior to the neovascular formation. The association between IGF-1 and microvascular impairment in AMD may be not limited to the neovascular stage but may be already evident in a less severe stage (intermediate) of the disease. This hypothesis is also corroborated by the observed grading in IGF-1 levels that were higher in the more advanced stages of the disease. IGF-1 levels in AMD may be considered a predisposing factor to the disease or, alternatively it may be a consequence of the degenerative processes which characterize AMD. Thus, these data are consistent with previous available data and may provide evidences for a pathogenetic or at least facilitating role of IGF-1 in AMD.
Furthermore, an indirect confirmation of the role of changes in circulating IGF-1 values in patients with intermediate and neovascular AMD is that, in these groups of patients, our results did not show a significant correlation with age, which instead was found in healthy patients and in the group with early stage of disease.
In a recent study Westwood and associates reported that IGF-1 plasma alterations are present in various neurodegenerative disorders. They demonstrated that lower serum levels of IGF-1 are associated with an increased risk of developing Alzheimer Disease (AD) dementia [23]. AMD is also characterized by retinal neurodegenerative processes [24] and previous studies have shown common pathogenetic features with AD [25]. Accordingly, is possible to suppose that IGF-1 is altered in various aging-related and neurodegenerative disorders [26]. As a result, the role of IGF-1 in neuronal inflammation needs to be elucidated.
It should be kept in mind that serum concentrations of IGF-1 are influenced by several factors, such as nutritional factors, energy and protein intake, and BMI. These factors may play as confounders in data analysis and interpretation. Our data also confirmed gender differences in IGF-1 levels that were previously observed [27].
Our study has several limitations including the cross-sectional nature of the study design with no longitudinal follow-up. In addition we didn’t evaluate IGF-1 levels in AMD patient affected by geographic atrophy, not clarifying whether the higher levels of IGF-1 in neovascular stage are linked to neovascular development or to the progression of neurodegenerative processes.
In conclusion circulating IGF-1 levels are significantly higher in patients affected by intermediate and neovascular AMD in comparison with control subjects. Although future studies with larger sample are needed, our results suggest IGF-1 as a possible contributing factor in the pathogenesis of this disease.
Methods
In this observational, prospective, controlled study we recruited consecutive patients of more than 60 years with a diagnosis of early AMD, intermediate AMD, neovascular AMD, and healthy controls examined at the Department of Ophthalmology, University of Catania, Catania, Italy, between January 2017 and May 2018. In each group, according to the power of the study, 28 male and 28 female patients were enrolled. The study was approved by the Institutional review board of the University of Catania. Written informed consent was obtained from all subjects enrolled in the study.
Exclusion criteria were diabetes and any systemic condition which could bias IGF-1 measurements, including any clinical condition which may have caused an elevation of systemic inflammatory markers, regardless of the cause that may have generated the rise. Patients in overweight or obese were excluded from the study (BMI above 29). Similarly patients with low body weight (BMI below 17.5) or patient with clinically evident sarcopenia were excluded. In addition, patients who had undergone to any previous intravitreal therapy, previous cataract surgery in the last six months or patients who had clinical evidence of other retinal and ocular disease were also excluded.
All patients enrolled were classified according to 4 stages classification of AMD from Age-related eye disease study (AREDS) [28]:
- No AMD (AREDS category 1) none or a few small drusen (<63 microns in diameter).
- Early AMD (AREDS category 2) any or all of the following: multiple small drusen, few intermediate drusen (63 to 124 microns in diameter), or RPE abnormalities.
- Intermediate AMD (AREDS category 3) any or all of the following: extensive intermediate drusen, and at least one large drusen (≥ 125 microns in diameter), or geographic atrophy not involving the center of the fovea.
- Neovascular AMD (AREDS category 4); any of the features of neovascular AMD.
All patients underwent an ophthalmic examination including: best corrected visual acuity (BCVA), applanation tonometry, slit-lamp biomicroscopic examination, Color fundus photography, optical coherence tomography (OCT) and, if needed, fluorescein angiography (FA) and indocyanine green angiography (ICGA).
Color fundus photography of the central retina was performed by Visucam (Carl Zeiss Meditec, Inc, Dublin, California, USA). At least two color fundus images of each eye were acquired capturing the central field of the retina within a 45° view. Images were defined as gradable, if they fulfilled the following quality criteria allowing for the assessment of AMD: sufficient brightness and color contrast as well as full macular region captured. Images were excluded from AMD grading, if they revealed obscuring lesions or lesions considered to be the result of a competing retinal disease hampering AMD grading. Gradable images were examined by an experienced and trained ophthalmology consultant (M.R.); questionable findings were discussed with a second trained grader (T.A.).
Spectral-domain OCT was carried out using the Spectralis HRA by Heidelberg (SD-OCT; Heidelberg Engineering, Heidelberg, Germany) FA and ICGA (Heidelberg retinal angiograph, Heidelberg Engineering, Heidelberg, Germany) were performed, in order to confirm the diagnoses in the neovascular AMD group.
Serum IGF-1 was measured by standard immunoassay in all patients. A 3 mL blood sample was drawn. This was obtained in the early morning at 08.00 after a 10 h overnight fasting. Prior to blood sampling patients were maintained in the supine position for 15 minutes. Samples were centrifuged, serum was aliquoted immediately and stored at -80°C in the central laboratory of our institution.
The primary outcome measure of our study was the evaluation of IGF-1 circulating levels in case and control groups in male and female patients. Secondary outcome was to evaluate the correlation between circulating IGF-1 levels and age in each group.
Statistical analysis
The sample size (at least 26 males and 26 females in each group) was determined from the results of our preliminary data to detect, with an alpha of 0.05 and a 90% power (two-tailed), a difference of 25 ng/ml in IGF-1 serum level between females with neovascular AMD and females with no AMD
The values of parameters in four groups were compared by ANOVA; if significant, comparison with baseline value was performed by Tukey HSD (honestly significant difference) test. In each group, correlation between IGF-1 levels and age was analyzed by Pearson's Correlation Coefficient. SPSS 21.0 (V.21, Armonk, NY, USA) was used for statistical analysis. P values < 0.05 was considered as statistically significant.
Conflicts of Interest
The authors have no conflicts of interest to declare.
Funding
No financial support was provided to this work.
References
- 1. Bressler NM. Age-related macular degeneration is the leading cause of blindness..... JAMA. 2004; 291:1900–01. https://doi.org/10.1001/jama.291.15.1900 [PubMed]
- 2. Wong WL, Su X, Li X, Cheung CM, Klein R, Cheng CY, Wong TY. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: a systematic review and meta-analysis. Lancet Glob Health. 2014; 2:e106–16. https://doi.org/10.1016/S2214-109X(13)70145-1 [PubMed]
- 3. Ferris FL
3rd , Wilkinson CP, Bird A, Chakravarthy U, Chew E, Csaky K, Sadda SR, and Beckman Initiative for Macular Research Classification Committee. Clinical classification of age-related macular degeneration. Ophthalmology. 2013; 120:844–51. https://doi.org/10.1016/j.ophtha.2012.10.036 [PubMed] - 4. Ferris FL
3rd , Fine SL, Hyman L. Age-related macular degeneration and blindness due to neovascular maculopathy. Arch Ophthalmol. 1984; 102:1640–42. https://doi.org/10.1001/archopht.1984.01040031330019 [PubMed] - 5. Reibaldi M, Longo A, Pulvirenti A, Avitabile T, Russo A, Cillino S, Mariotti C, Casuccio A. Geo-Epidemiology of Age-Related Macular Degeneration: New Clues Into the Pathogenesis. Am J Ophthalmol. 2016; 161:78–93.e1, 2. https://doi.org/10.1016/j.ajo.2015.09.031 [PubMed]
- 6. Longo A, Casuccio A, Pani L, Avitabile T, Cillino S, Uva MG, Bonfiglio V, Russo A, Parisi G, Cennamo G, Furino C, Parravano M, Xoxi E, Reibaldi M. Association of neovascular age-related macular degeneration with month and season of birth in Italy. Aging (Albany NY). 2016; 9:133–41. https://doi.org/10.18632/aging.101137 [PubMed]
- 7. Wong TY, Chakravarthy U, Klein R, Mitchell P, Zlateva G, Buggage R, Fahrbach K, Probst C, Sledge I, Sledge I. The natural history and prognosis of neovascular age-related macular degeneration: a systematic review of the literature and meta-analysis. Ophthalmology. 2008; 115:116–26. https://doi.org/10.1016/j.ophtha.2007.03.008 [PubMed]
- 8. Witmer AN, Vrensen GF, Van Noorden CJ, Schlingemann RO. Vascular endothelial growth factors and angiogenesis in eye disease. Prog Retin Eye Res. 2003; 22:1–29. https://doi.org/10.1016/S1350-9462(02)00043-5 [PubMed]
- 9. Brown DM, Regillo CD. Anti-VEGF agents in the treatment of neovascular age-related macular degeneration: applying clinical trial results to the treatment of everyday patients. Am J Ophthalmol. 2007; 144:627–37. https://doi.org/10.1016/j.ajo.2007.06.039 [PubMed]
- 10. Ferrara N, Damico L, Shams N, Lowman H, Kim R. Development of ranibizumab, an anti-vascular endothelial growth factor antigen binding fragment, as therapy for neovascular age-related macular degeneration. Retina. 2006; 26:859–70. https://doi.org/10.1097/01.iae.0000242842.14624.e7 [PubMed]
- 11. Reibaldi M, Pulvirenti A, Avitabile T, Bonfiglio V, Russo A, Mariotti C, Bucolo C, Mastropasqua R, Parisi G, Longo A. Pooled estimates of incidence of endophthalmitis after intravitreal injection of anti-vascular endothelial growth factor agents with and without topical antibiotic prophylaxis. . Retina. 2018; 38:1–11. https://doi.org/10.1097/IAE.0000000000001583 [PubMed]
- 12. Haddad S, Chen CA, Santangelo SL, Seddon JM. The genetics of age-related macular degeneration: a review of progress to date. Surv Ophthalmol. 2006; 51:316–63. https://doi.org/10.1016/j.survophthal.2006.05.001 [PubMed]
- 13. Jonas JB, Tao Y, Neumaier M, Findeisen P. Monocyte chemoattractant protein 1, intercellular adhesion molecule 1, and vascular cell adhesion molecule 1 in exudative age-related macular degeneration. Arch Ophthalmol. 2010; 128:1281–86. https://doi.org/10.1001/archophthalmol.2010.227 [PubMed]
- 14. Jonas JB, Tao Y, Neumaier M, Findeisen P. Cytokine concentration in aqueous humour of eyes with exudative age-related macular degeneration. Acta Ophthalmol. 2012; 90:e381–88. https://doi.org/10.1111/j.1755-3768.2012.02414.x [PubMed]
- 15. Kramer M, Hasanreisoglu M, Feldman A, Axer-Siegel R, Sonis P, Maharshak I, Monselise Y, Gurevich M, Weinberger D. Monocyte chemoattractant protein-1 in the aqueous humour of patients with age-related macular degeneration. Clin Experiment Ophthalmol. 2012; 40:617–25. https://doi.org/10.1111/j.1442-9071.2011.02747.x [PubMed]
- 16. Samani AA, Yakar S, LeRoith D, Brodt P. The role of the IGF system in cancer growth and metastasis: overview and recent insights. Endocr Rev. 2007; 28:20–47. https://doi.org/10.1210/er.2006-0001 [PubMed]
- 17. Balasubramanian P, Longo VD. Growth factors, aging and age-related diseases. Growth Horm IGF Res. 2016; 28:66–68. https://doi.org/10.1016/j.ghir.2016.01.001 [PubMed]
- 18. Cha DM, Woo SJ, Kim HJ, Lee C, Park KH. Comparative analysis of aqueous humor cytokine levels between patients with exudative age-related macular degeneration and normal controls. Invest Ophthalmol Vis Sci. 2013; 54:7038–44. https://doi.org/10.1167/iovs.13-12730 [PubMed]
- 19. Machalinska A, Safranow K, Dziedziejko V, Mozolewska-Piotrowska K, Paczkowska E, Klos P, Pius E, Grymula K, Wiszniewska B, Karczewicz D, Machalinski B. Different populations of circulating endothelial cells in patients with age-related macular degeneration: a novel insight into pathogenesis. Invest Ophthalmol Vis Sci. 2011; 52:93–100. https://doi.org/10.1167/iovs.10-5756 [PubMed]
- 20. Lambooij AC, van Wely KH, Lindenbergh-Kortleve DJ, Kuijpers RW, Kliffen M, Mooy CM. Insulin-like growth factor-I and its receptor in neovascular age-related macular degeneration. Invest Ophthalmol Vis Sci. 2003; 44:2192–98. https://doi.org/10.1167/iovs.02-0410 [PubMed]
- 21. Economou MA, Wu J, Vasilcanu D, Rosengren L, All-Ericsson C, van der Ploeg I, Menu E, Girnita L, Axelson M, Larsson O, Seregard S, Kvanta A. Inhibition of VEGF secretion and experimental choroidal neovascularization by picropodophyllin (PPP), an inhibitor of the insulin-like growth factor-1 receptor. Acta Ophthalmol. 2008; 86 Thesis 4:42–49. https://doi.org/10.1111/j.1755-3768.2008.01185.x [PubMed]
- 22. Grant MB, Mames RN, Fitzgerald C, Ellis EA, Aboufriekha M, Guy J. Insulin-like growth factor I acts as an angiogenic agent in rabbit cornea and retina: comparative studies with basic fibroblast growth factor. Diabetologia. 1993; 36:282–91. https://doi.org/10.1007/BF00400229 [PubMed]
- 23. Westwood AJ, Beiser A, Decarli C, Harris TB, Chen TC, He XM, Roubenoff R, Pikula A, Au R, Braverman LE, Wolf PA, Vasan RS, Seshadri S. Insulin-like growth factor-1 and risk of Alzheimer dementia and brain atrophy. Neurology. 2014; 82:1613–19. https://doi.org/10.1212/WNL.0000000000000382 [PubMed]
- 24. Zucchiatti I, Parodi MB, Pierro L, Cicinelli MV, Gagliardi M, Castellino N, Bandello F. Macular ganglion cell complex and retinal nerve fiber layer comparison in different stages of age-related macular degeneration. Am J Ophthalmol. 2015; 160:602–607.e1. https://doi.org/10.1016/j.ajo.2015.05.030 [PubMed]
- 25. Ong SS, Proia AD, Whitson HE, Farsiu S, Doraiswamy PM, Lad EM. Ocular amyloid imaging at the crossroad of Alzheimer’s disease and age-related macular degeneration: implications for diagnosis and therapy. J Neurol. Epub ahead of print. https://doi.org/10.1016/j.ajo.2015.05.030 [PubMed]
- 26. Pennington KL, DeAngelis MM. Epidemiology of age-related macular degeneration (AMD): associations with cardiovascular disease phenotypes and lipid factors. Eye Vis (Lond). 2016; 3:34. https://doi.org/10.1186/s40662-016-0063-5 [PubMed]
- 27. Austad SN, Bartke A. Sex Differences in Longevity and in Responses to Anti-Aging Interventions: A Mini-Review. Gerontology. 2015; 62:40–46. https://doi.org/10.1159/000381472 [PubMed]
- 28. Age-Related Eye Disease Study Research Group. A randomized, placebo-controlled, clinical trial of high-dose supplementation with vitamins C and E, beta carotene, and zinc for age-related macular degeneration and vision loss: AREDS report no. 8. Arch Ophthalmol. 2001; 119:1417–36. https://doi.org/10.1001/archopht.119.10.1417 [PubMed]



